This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Individualized 'coaching' for better chronic pain care
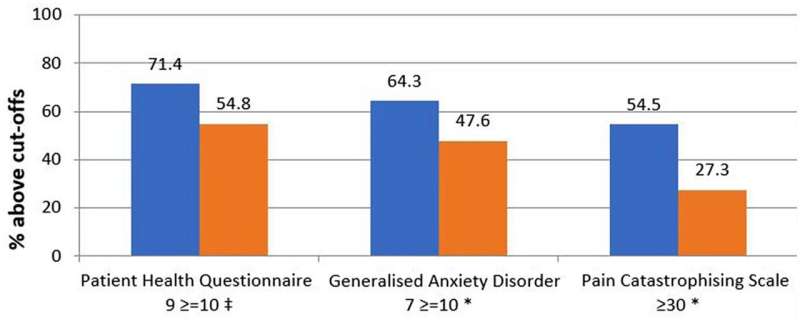
Chronic pain affects millions of people worldwide and is a leading cause of disability and health care use.
A new study led by Flinders University has shown that timely, affordable, integrated and individualized "coaching" can help people living with chronic pain to improve their self-management and understanding of ways to better manage their pain.
A novel telehealth program developed by Flinders University and SA Health experts shows the potential for non-mental health professionals—in tandem with medical and allied health experts—to help those living with chronic pain to access specialized support that can make a difference and reduce suffering.
The program also provides access to care and support for people living outside of metro areas who may have to otherwise wait years to see a pain specialist, says Flinders University Behavioral Health expert Paula Redpath, from the College of Medicine and Public Health.
A pilot study of the "Rethinking Pain" guided self-help program in South Australia showed it to be a promising model for providing specialized information and support through supervised "coaches" who worked with people with chronic pain to increase their understanding of their condition and improve their self-management.
"Accessing care and support for chronic pain is difficult, time-consuming and costly, particularly for people living in rural and remote areas," says Ms. Redpath, Behavioral Health Discipline Lead at Flinders University.
"Chronic pain is a complex condition that often requires specialized, multidisciplinary teams to provide effective and integrated care.
"Once a person understands helpful ways to manage their chronic pain, they can choose what strategies they want to use to self-manage.
"The coaches guide and assist people with these strategies, which they can then take away and use."
The program can be offered via telehealth or in person and involves goal setting, pain conceptualization, activity scheduling, psycho-education, pacing and cognitive strategies, with evaluation of the program outcomes demonstrating significant improvement in patients' reported independence and quality of life.
"Coaches can become part of the multidisciplinary team and support patients by providing them with information and strategies to manage their chronic pain. This can relieve pressure on higher-trained health and medical professionals, allowing them to concentrate on more complex care," says Flinders University academic Dr. Peter Herriot from the SA Health Southern Adelaide Local Health Network (SALHN) Pain Management Unit, who supervised the trial.
"This evidence-based program has the potential to not only improve access to care for people who are living with chronic pain but also to be scaled up and adopted across a variety of health care settings."
The guided self-help (GSH) program, developed by Flinders University experts, was delivered by supervised postgraduate students from the University's Master of Cognitive Behavior Therapy course who undertook placement at SA Health's Pain Management Unit at Flinders Medical Center, Bedford Park.
An estimated 1 in 5 Australians aged 45 and over have chronic pain. The annual direct and indirect costs of chronic pain is reported to be an estimated $139 billion—including loss of productivity and loss of quality of life.
Wider implementation of programs such as "Rethinking Pain" is important to expand and improve care options for people living with chronic pain, adds Ms. Redpath.
"Disseminating this specialist knowledge to a diversified health workforce and peers in the community and through primary care services may also reduce demand for psychiatrists and psychologists whose services are limited and hard to access."
People living with chronic pain can also experience significant physical and emotional impacts, including on sleep quality and well-being as well as impacts on employment. Access to adequate support services can be difficult due to social disadvantage.
The work is published in the journal Pain and Therapy.
More information: Paula Redpath et al, Guided Self-Help for People with Chronic Pain: Integrated Care in a Public Tertiary Pain Clinic—A Pilot Study, Pain and Therapy (2023). DOI: 10.1007/s40122-022-00464-z





















