This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Study finds underperforming organ procurement organizations contribute to nationwide shortage
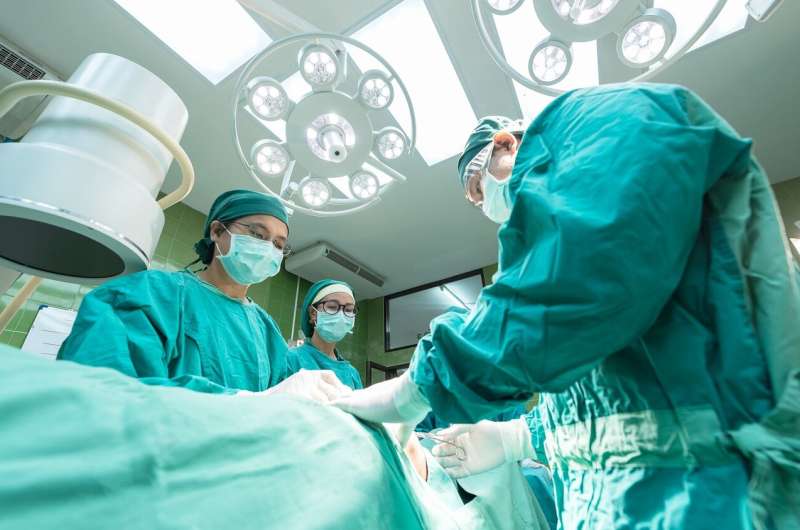
The number of potential organ donors in the United States could solve the shortage for most organs, but many organs are not recovered due to performance variations in the opaque organ procurement organization process, according to a just-published study with first and corresponding authors from Vanderbilt University Medical Center.
The study, "Variability in Organ Procurement Organization Performance by Individual Hospital in the United States," published in JAMA Surgery, includes VUMC authors Wali Johnson, MD, and Seth Karp, MD, H. William Scott Jr. Professor, chair of the Section of Surgical Sciences and director of the Vanderbilt Transplant Center.
"With better government oversight and organ procurement organization performance, we have the potential to nearly eliminate deaths on transplant waiting lists," Karp said.
More than 11,000 waitlisted patients died or became too sick for a transplant in 2021 alone, the study states, highlighting the critical need to increase the supply of donor organs. To compare donor potential to actual donors, researchers performed a retrospective cross-sectional analysis across 13 hospitals covered by two organ procurement organizations (OPOs) in 2017 and 2018.
By reviewing 2,008 medical records of deceased patients to make estimates of 8,925 total patient deaths, the study identified patients who had deaths with causes consistent with donation as well as the number of ventilated patients. It then compared that to the number of patients who actually donated organs. It considered the number of ventilated patient referrals and center acceptance practices. Lastly, it compared the success of obtaining donations of one OPO to the other.
The study found 931 potential organ donors compared to 242 actual donors, suggesting large unmet potential to increase the organ supply. It also found that one OPO was "surprisingly" much more successful in obtaining organs; one recovered 18.8% of potential donors and one recovered 48.2%. The hospitals and organ procurement organizations were deidentified for purposes of analysis.
"It becomes clear that even a modest increase in donors could solve the current nonrenal organ shortage and decrease the time waiting to receive a deceased-donor kidney," the article states.
To reach these findings, researchers looked at all aspects that must occur before an organ can be successfully obtained and transplanted. First, a hospital identifies a patient who died in the right circumstances to become a donor and refers the patient to the OPO. Next the OPO evaluates the referral, determines if donation is possible and obtains family or first-person consent. At that stage, the hospital and OPO manage the donor while the OPO determines which centers' recipients are compatible matches for organs. Once a specific center accepts an organ, a surgical team removes the organ and returns it to the center for transplant.
The study found that OPO performance was not related to transplant center acceptance practices, and only moderately related to how many ventilated patients hospitals referred. It found OPO performance was the largest factor in how many organs were recovered but could not determine why because the authors were not permitted access to detailed OPO records.
In conclusion, the authors propose a "relatively easy" solution: Make OPO data available to oversight bodies and researchers. The Centers for Medicare & Medicaid Services (CMS) already require OPOs to collect data on the number of hospital deaths, results of death record reviews and number and timeliness of referral calls from hospitals. The authors encourage CMS to require further transparency in OPO data.
More information: Wali Johnson et al, Variability in Organ Procurement Organization Performance by Individual Hospital in the United States, JAMA Surgery (2023). DOI: 10.1001/jamasurg.2022.7853