This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Clues to the cause of chronic gut pain
New insights into chronic gut pain offer hope for improved treatments for irritable bowel syndrome and anxiety treatment.
A research team led by Flinders University Professor Stuart Brierley, based at the SA Health and Medical Research Institute, with Nobel Laureate Professor David Julius, Professor Holly Ingraham and Dr. James Bayrer at the University of California San Francisco, has shown evidence of a specific pathway of cells and nerves linking the gut to the brain that may be responsible for the chronic gut pain.
Chronic gut pain is commonly experienced by 11% of the global population currently living with irritable bowel syndrome (IBS) and associated psychological conditions, including anxiety and depression.
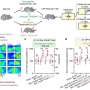
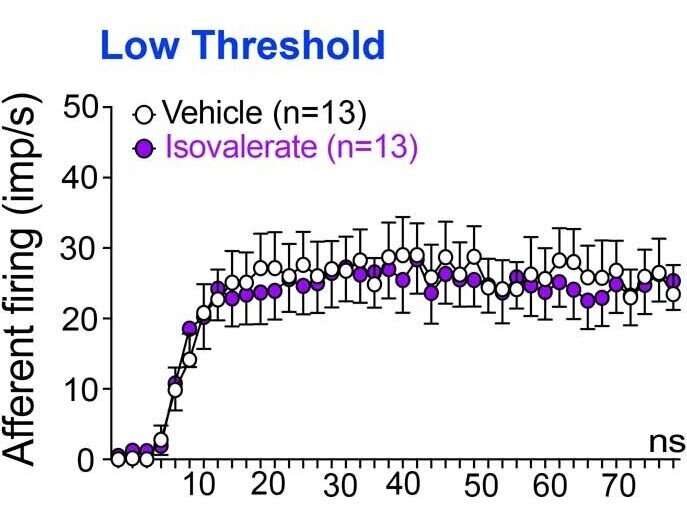
Described in a new article in Nature, the team used genetic and pharmacologic tools in pre-clinical models to manipulate signals between gut epithelial cells and associated nerve fibers to determine how this pathway stimulates chronic gut pain and anxiety.
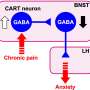
"We've found that the gut microbiome produces short chain fatty acids that act on the lining of the gut and trigger a particular cell type to release neurotransmitters," says Professor Brierley.
"The nerves connecting to those cells become active and directly send pain signals to the brain via the gut-brain axis. Activation of these nerves also increases anxiety indicators.
"This mechanism is chronically overactive in females, which could explain why two-thirds of those who experience IBS are women and why IBS patients report symptoms of chronic gut pain and anxiety."
The research suggests IBS, anxiety and depression can all be driven by signaling within the intestinal tract and people with overactive communication between the gut and brain are more susceptible to experiencing pain.
Professor Brierley says added stress can make the symptoms even worse by further activating these mechanisms in the gut.
"There's a variety of ways in which your susceptibility to pain can be altered on a daily-basis.
"Stress, infections, changes in diet and disruptions to the microbiome caused by medications, such as antibiotics, can mess with the way your gut signals to your brain."
Researchers are striving to address the current lack of treatments for chronic gut pain and anxiety and now that the mechanisms involved in driving these conditions have been discovered, specific interventions can be developed to block communication between the cells and nerves responsible.
"Theoretically we should be able to find a way to stop gut pain at the source and simultaneously reduce feelings of anxiety.
"These future interventions are likely to include drug treatments, microbiome treatments and diet-based treatments."
More information: James R. Bayrer et al, Gut enterochromaffin cells drive visceral pain and anxiety, Nature (2023). DOI: 10.1038/s41586-023-05829-8