This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
proofread
Study identifies major risk factors of pulmonary tuberculosis in patients with pneumoconiosis in China
Pneumoconiosis comprises a group of heterogeneous lung diseases resulting from the inhalation of mineral dust. It is an occupational hazard with significant economic and social implications. Notably, patients with pneumoconiosis have an elevated risk of contracting pulmonary tuberculosis (PTB). Unfortunately, pneumoconiosis has a strong presence in China. However, extensive population-based studies on the prevalence of PTB in patients with pneumoconiosis have not been conducted in China since almost three decades.
To bridge this gap, a team of researchers led by Dr. Huanqiang Wang from the Chinese Center for Disease Control and Prevention, China, recently conducted a study to understand the epidemiological characteristics of PTB and its risk factors in patients with pneumoconiosis in China. Their study was published in the Chinese Medical Journal.
In 2019, China issued the "National Action Plan to Stop Tuberculosis". Elaborating on the reasons underlying such an initiative, Dr. Wang says, "By the end of 2021, a total of 915,000 cumulative cases of pneumoconiosis had been reported in China, with an average of 13,000 newly diagnosed patients annually in the past 10 years"
"China bears the most significant burden of pneumoconiosis across the world. Pulmonary tuberculosis (PTB) is a respiratory infectious disease caused by Mycobacterium tuberculosis (M. tuberculosis) infection, which seriously endangers people's health. It is one of the leading causes of morbidity and death worldwide and is listed as a significant infectious disease in China."
In order to learn more about pneumoconiosis and its association with PTB, the research team launched a questionnaire-based survey targeted towards patients of different backgrounds. Participating patients met the conditions of a clear history of exposure to mineral dust, a chest X-ray showing abnormal appearance in the posteroanterior view, and some disease-related symptoms.
Moreover, the research team ensured that other pulmonary diseases were differentially diagnosed as per the established protocol. Next, qualified occupational disease physicians and nurses interacted with these patients. The pneumoconiosis cases included patients with official occupational disease diagnostic certificates and patients clinically diagnosed by qualified physicians according to the GBZ 70-2015 Diagnosis of Occupational Pneumoconiosis.
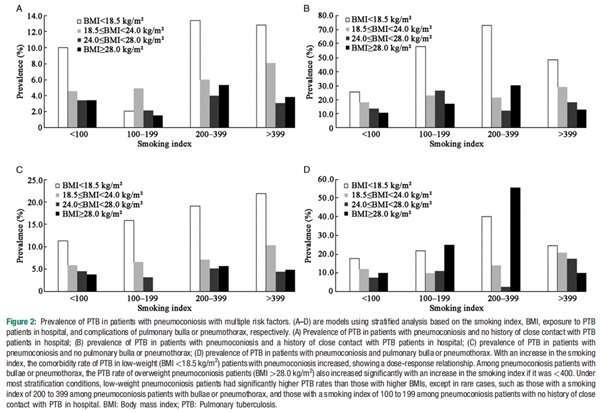
The findings of the survey suggested that the prevalence of PTB in patients with pneumoconiosis (n = 10,137) was as high as 7.5%. The average dust exposure time was found to be 19 ± 10 years and the average age at which patients with pneumoconiosis commenced smoking was 23 ± 8 years. Both smoking and alcohol consumption were found to be higher in patients from rural neighborhoods as compared to patients from urban neighborhoods.
On conducting statistical analyses, the team found that risk factors also included in-hospital exposure to other patients with PTB. In addition, smoking, low body mass index, low personal income/unemployment, and years of exposure to dust were statistically significant risk factors for the development of PTB.
Additional relevant risk factors included lack of work-related injury insurance (WRII), being born in a rural area, living in western regions, household exposure to patients with PTB, complications of pulmonary bullae or pneumothorax, and hospitalization history. Among all the rural patients, former alcohol drinkers exhibited a relatively higher PTB risk. All of the above associations persisted even after adjusting for confounding factors such as age, sex, and pneumoconiosis type.
The statistically determined population attributable fraction (PAF)—the contribution of a risk factor to the burden of disease— was 13.2%, 12.5%, and 11.6% for birth in a rural area, lack of WRII, and in-hospital exposure to patients with PTB, respectively.
"The World Health Organization (WHO) Commission on Social Determinants of Health (CSDH) believes that health inequity caused by inequitable social status and resource allocation is the most fundamental cause of social determinants affecting society's health status. Our study is the first to systematically apply the concept and model of CSDH to analyze PTB's social determinants and risk factors in patients with pneumoconiosis. We also calculated the PAFs of significant risk factors for PTB with pneumoconiosis for the first time," adds senior author Dr. Tao Li from the Chinese Center for Disease Control and Prevention.
The authors are hopeful that with effective measures such as the promotion, prevention, diagnosis, control, and treatment of pneumoconiosis and enhanced social security, the incidence of PTB will diminish considerably in China over the years.
More information: Huanqiang Wang et al, Epidemiological characteristics of pulmonary tuberculosis in patients with pneumoconiosis based on its social determinants and risk factors in China: a cross-sectional study from 27 provinces, Chinese Medical Journal (2023). DOI: 10.1097/CM9.0000000000002486