This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Study reveals a driver of brain cell damage in neurodegeneration
Scientists have long known that the complement cascade, a set of immune system proteins, protects against infection in the body. But in recent years, researchers have uncovered new roles for the system in the brain, including helping to whittle down connections between brain cells, or synapses, to help shape the nervous system early in life. They've also found that the pathway can become dysregulated in the adult brain, leading to cell damage and cell death seen in conditions such as Alzheimer's disease and schizophrenia. But researchers didn't know how exactly that happens.
A new study led in part by scientists in the Stanley Center for Psychiatric Research at the Broad Institute of MIT and Harvard has identified the first known regulator of the complement system in the adult brain: the neuronal pentraxin protein Nptx2. Loss of Nptx2 leaves the cascade unchecked, exacerbating synapse destruction. In models of neurodegeneration, the researchers overcame these effects by boosting Nptx2 levels or blocking complement protein in cells, suggesting that therapeutic strategies targeting the complement system could prevent or even reverse damage to brain cells in neurodegenerative disease.
The work appears in the March 29 issue of Science Translational Medicine.
"There's still a lack of understanding of precisely what factors and sequence of events drive neurodegenerative disorders," said study co-senior author Borislav Dejanovic, a scientist in the Stanley Center who is now director of Vigil Neuroscience. "Findings like this help us learn what mediates the synapse loss and cognitive decline that is devastating for patients and their families."
"This study contributes to the emerging picture of the complement cascade's role across a range of neurological disorders," said co-senior author and Broad core institute member Morgan Sheng, who is also co-director of the Stanley Center, a professor of neuroscience in MIT's Department of Brain and Cognitive Sciences, and an affiliate of the Picower Institute for Learning and Memory. "In the Stanley Center, we're working to elucidate the common mechanisms among diverse brain disorders, to reveal unexpected connections and promising therapeutic avenues that could one day benefit patients."
Dejanovic and Sheng led the work along with co-senior author Paul Worley, a professor of neuroscience at the Johns Hopkins University School of Medicine.
An overzealous cascade
In the brain, complement proteins bind to synapses as "eat me" signals, alerting immune cells called microglia to engulf and destroy the cellular connections. Scientists have speculated that the process is normally tightly regulated in the central nervous system to protect healthy cells from damage, but they hadn't yet found any molecules in the adult brain that regulate the pathway.
The researchers proposed that members of the pentraxin family of proteins are possible candidates, because these proteins are known to regulate complement activity elsewhere in the body. The scientists zeroed in on the pentraxin called Nptx2, which is secreted by excitatory neurons and is a biomarker for a range of neurological disorders. In patients with Alzheimer's disease, frontotemporal dementia, schizophrenia, and Down's syndrome, Nptx2 is depleted in the cerebrospinal fluid that surrounds the brain and spinal cord.
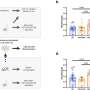
In their study, the researchers saw that Nptx2 directly and specifically binds and inhibits the activity of C1q, the initiating factor of the complement cascade.
Further, in an animal model lacking Nptx2, they found increased activity of the complement system along with destruction of synapses by microglia. When they eliminated C1q in these animals through genetic deletion or antibody blocking, synapses in the brain tissue recovered.
In an animal model of neurodegeneration marked by overactive microglia and elevated complement activity, boosting the production of Nptx2 in certain brain cells led to a decrease in complement activity and reversed the loss of synapses.
Human factors
To test whether this pattern might occur in humans, too, the researchers measured the levels of complement and pentraxin proteins in cerebrospinal fluid from patients with genetic frontotemporal dementia, both before and after symptoms developed. Levels of C1q and C3b, an activated complement protein further down the cascade, were higher in symptomatic patients than in presymptomatic genetic carriers, and levels of Nptx2 were lower. The team also observed that levels of Nptx2 bound to C1q were reduced in symptomatic patients, suggesting that abundant unbound C1q could be driving synapse loss and leading to symptoms of dementia.
"The findings help explain how a decrease of this biomarker could lead to synapse loss," said Dejanovic. "When Nptx2 decreases, complement is no longer constrained."
The work bolsters the therapeutic strategy of inhibiting the complement pathway, which could one day improve symptoms for patients with neurodegenerative or neuroinflammatory disorders—an approach that is currently being explored by the pharmaceutical industry.
In the meantime, the researchers will continue to explore how this molecular system is controlled in health and in other central nervous system disorders, such as bipolar disorder.
More information: Jiechao Zhou et al, The neuronal pentraxin Nptx2 regulates complement activity and restrains microglia-mediated synapse loss in neurodegeneration, Science Translational Medicine (2023). DOI: 10.1126/scitranslmed.adf0141