This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Clinical trial improves neurocognitive outcomes for childhood craniopharyngioma

St. Jude Children's Research Hospital is reporting phase 2 clinical trial results treating the brain tumor craniopharyngioma with proton therapy. The researchers found a similar survival rate between more targeted proton therapy and photon therapy but improved neurocognitive outcomes with the proton therapy. The clinical trial may set the new "gold standard" for pediatric craniopharyngioma treatment. The study was published today in Lancet Oncology.
"The trial is an unprecedented study comparing proton and photon therapy for craniopharyngioma," said principal investigator Thomas E. Merchant, D.O., Ph.D., St. Jude Department of Radiation Oncology chair. "We found a benefit for cognitive outcomes in patients treated with proton therapy, while maintaining a high survival rate."
Setting a new 'gold standard'
"The results of this prospective clinical trial are likely to set a new 'gold standard' for the treatment of childhood craniopharyngioma," said co-author Frederick Boop, M.D., St. Jude Department of Surgery.
The study is the first prospective longitudinal study comparing proton therapy to 3D conformal photon therapy in children with this tumor.
"We have long recognized a theoretical benefit [of this approach] but now have proof that proton therapy causes fewer cognitive side effects than photons," Boop explained.
The overall survival, progression-free survival and cognitive outcomes recognized five years after treatment in this study show benefits over other treatment approaches.
Proton therapy spares the healthy brain
Craniopharyngioma is a rare brain tumor that forms in the central region of the brain, making it difficult to treat without exposing surrounding healthy brain tissue to radiation. Conventional radiation therapy, called photon therapy, has raised the five-year survival rate for this cancer to 90%. However, patients may experience treatment-related neurocognitive late effects.
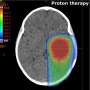
Photons (X-rays) pass through the tumor, whereas protons (a charged particle and the nucleus of the hydrogen atom) can be directed to stop within the tumor. This is why proton therapy spares normal brain tissue and reduces collateral effects. This St. Jude trial highlights the therapeutic advantage for children and adolescents with craniopharyngioma for the first time.
"Proton therapy is a very focused treatment, which exposes the normal brain tissue to less radiation than photon therapy," Merchant said. "It's that simple. The parts of the brain that have been spared make the difference here. What's unique about craniopharyngioma is that it's consistently located in the central part of the brain and intimately associated with the central blood supply, optic nerves and chiasm, hypothalamic-pituitary axis, and other critical areas associated with cognitive outcomes."
Comparing protons vs. photons
While proton therapy was created to lower radiation exposure to the brain, no previous clinical trials for children with brain tumors had prospectively shown its functional benefit compared to photon therapy in a single tumor type.
The St. Jude group compared proton therapy results over five years to a historical control group treated with photon therapy at the hospital. The five-year progression-free survival was 93.6% in the proton group. This result was not statistically significantly different from photon therapy (~90.0%), but it did show proton therapy maintained the same high survival rate.
For neurocognitive outcomes, proton therapy was superior to photon therapy. Patients treated with photon therapy experienced an average loss of 1.09 Intelligence Quotient (IQ) points more than those treated with proton therapy every year for the five years of the study. Similarly, patients exposed to photon therapy lost 1.48 adaptive behavior points, a parental report of self-care skills—more than those treated with proton therapy—each year. The cognitive deficits of those treated with proton therapy were stable by the end of the study.
"Improved intellectual and adaptive functioning afforded by proton therapy, in the context of maintained high survival rates, is a huge win for patients diagnosed with craniopharyngioma and their families," said co-author Heather Conklin, Ph.D., St. Jude Department of Psychology and Biobehavioral Sciences. "As survival rates continue to improve for children treated for brain tumors, it is imperative we optimize quality of life after treatment."
"These results could be practice changing if they convince caregivers to recommend proton beam therapy over radical surgery or referral of patients using proton beam therapy instead of radiotherapy using photons," Merchant said. "The results of this trial are important for the field of pediatric radiation oncology because they realize a goal to show a benefit of proton therapy over photon therapy. We've been waiting years for these results."
More information: Thomas E Merchant et al, Proton therapy and limited surgery for paediatric and adolescent patients with craniopharyngioma (RT2CR): a single-arm, phase 2 study, The Lancet Oncology (2023). DOI: 10.1016/S1470-2045(23)00146-8