This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Safety of GP prescribing in England was not adversely affected by the pandemic, says study
Researchers from the Universities of Nottingham and Oxford have found that despite substantial disruption to primary care services, the safety of GP prescribing in England was largely unaffected by the COVID-19 pandemic.
The study, published in the BMJ Medicine, is the most comprehensive assessment of medication safety during the COVID-19 pandemic in England, covering 95% of the population.
The research also demonstrates the power of analyzing NHS GP data on a national scale to generate insights on service delivery.
The findings are based on the application of the 13 national PINCER prescribing safety indicators to the electronic health records of almost 57 million NHS patients in England between September 2019 and September 2021 using the OpenSAFELY platform.
PINCER is an evidence-based, pharmacist-led complex intervention to identify and correct hazardous prescribing in primary care. PINCER was rolled out nationally to GP practices in England between 2018 and 2021 by PRIMIS at the University of Nottingham in collaboration with the Academic Health Science Network. PRIMIS is a specialist team of health informaticians within the School of Medicine at the University of Nottingham providing expert advice on the intelligent use of primary care data to the NHS, academics, and industry partners.
OpenSAFELY is a secure, transparent open-source software platform for the analysis of electronic health records developed in collaboration with GP software suppliers TPP and EMIS Health to address urgent COVID-19 research questions.
The COVID-19 pandemic disrupted the delivery of primary care services within the NHS in the UK from March 2020, with a 30% reduction in GP consultations, a 74% reduction in routine referrals and a 43% reduction in urgent cancer referrals. The extent of disruption varied by clinical context, though most primary care services were restored by September 2020.
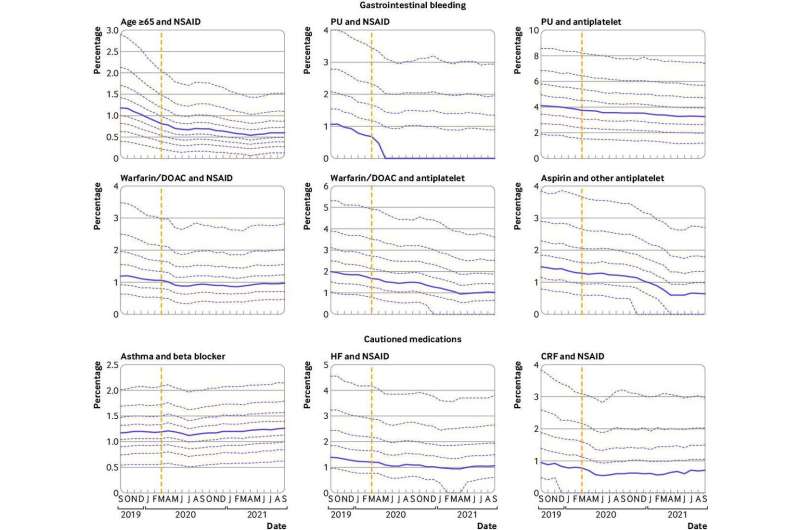
Monthly trends and between-practice variation for compliance with the PINCER indicators were investigated. Findings showed that 1,813,058 (3.1%) patients registered across 6,367 practices were identified as being at risk of at least one potentially hazardous prescribing event at any point during the study period.
Hazardous prescribing remained largely unchanged during the COVID-19 pandemic, with no evidence of increases in indicators of harm as captured by the PINCER indicators. There were transient delays in blood test monitoring for some medications, particularly ACE inhibitors. However, all indicators exhibited substantial recovery by September 2021.
Kerry Oliver, PRIMIS managing director at the University of Nottingham, said "This study underlines the success of the national roll out of the PINCER Intervention, which harnessed the power of data and feedback to support positive, sustained change, of which PRIMIS has a long history of supporting."
Brian MacKenna, director for NHS Service Analytics at Oxford's Bennett Institute for Applied Data Science, added, "The NHS has a phenomenal coverage and quality of data that can be used to help answer important questions to inform our response to COVID-19. While using this data, it is important that we keep patient's data secure. That's why we have built OpenSAFELY, a new highly secure model that takes the analytics to where the data already resides."
Dr. Sarah Rodgers, PRIMIS head of research services, said, "Despite all the challenges that general practice faced during the COVID-19 pandemic, prescribing safety obviously remained high on the agenda. These findings are testament to the hard work and dedication of the pharmacists, pharmacy technicians and GPs working in primary care during this time."
More information: Louis Fisher et al, Changes in medication safety indicators in England throughout the covid-19 pandemic using OpenSAFELY: population based, retrospective cohort study of 57 million patients using federated analytics, BMJ Medicine (2023). DOI: 10.1136/bmjmed-2022-000392