People who walk on a treadmill even years after stroke damage can significantly improve their health and mobility, changes that reflect actual "rewiring" of their brains, according to research spearheaded at Johns Hopkins.
"This is great news for stroke survivors because results clearly demonstrate that long-term stroke damage is not immutable and that with exercise it's never too late for the brain and body to recover," says Daniel Hanley, M.D., professor of neurology at the Johns Hopkins University School of Medicine.
The study's results, published in Stroke: Journal of the American Heart Association, suggest that patients' brains may retain the capacity to rewire through a treadmill exercise program months or years after conventional physical therapy has ended.
The research was conducted by scientists at Johns Hopkins, the University of Maryland, and the Department of Veterans Affairs Maryland VA Medical Center at their Geriatric Research, Education, and Clinical Center (GRECC). Researchers at the GRECC, led by Richard F. Macko, M.D., and Andrew P. Goldberg, M.D., have developed treadmill therapy for stroke patients over the past decade. Investigators at all three institutions combined efforts to recruit 71 patients who had a stroke at least six months earlier, with an average time lapse of nearly four years. At the study's onset, half of the subjects could walk without assistance, while the rest used a cane, a walker or a wheelchair.
All of the subjects, separated into two random groups regardless of disability, were tested for mobility and aerobic capacity (also known as VO2 peak), a measure of cardiac fitness. Thirty-two patients drawn equally from both groups underwent functional magnetic resonance imaging (fMRI) to assess brain activity linked to moving their legs in a walking motion.
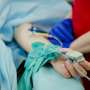
One group then participated in an exercise program that principally involved walking on a treadmill three times a week for up to 40 minutes, assisted by a supporting sling and tether if needed. Physical therapists assigned to each subject increased the intensity of the workouts over time by increasing the treadmills' speed and incline, though the workouts never taxed the patients beyond a moderate level of 60 percent VO2 peak.
With the second group of patients, therapists assisted the patients in performing stretching exercises for the same period of time.
After six months, patients were again tested for walking speed and VO2 peak, and the same group who had undergone fMRI was rescanned. Walking speed for the treadmill group increased 51 percent compared to about 11 percent faster for those in the stretching group. Ground walking speed among the treadmill exercisers increased 19 percent, compared to about 8 percent for the stretchers. The treadmill exercisers also were significantly more fit at study completion, with VO2 peak increasing by about 18 percent. VO2 peak decreased slightly in the stretching group.
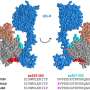
Hoping to find evidence that improved brain activity was responsible for the results, the investigators analyzed the brain scans and found markedly increased metabolic activity in brainstem areas associated with walking among all the treadmill exercisers. Brain scans of patients in the stretching group showed no such changes.
"This suggests that the brain is responsible for the improvement we saw in patients' walking ability. It seems to be recruiting other regions to take on the job of areas damaged by stroke," says Andreas Luft, M.D., a visiting researcher who worked with all three institutions who conducted this study. Luft is currently a stroke attending physician and professor of neurorehabilitation at the University of Zurich in Switzerland.
Those patients with the most improvement in walking showed the strongest change in brain activity, though the researchers don't yet know whether these brain changes were caused by more walking or whether participants walked better because brain activity in these key areas increased. This question will be the focus of a future study.
Hanley says stroke patients are typically told to "learn to live with" their disabilities, unlike heart attack patients and others who are often prescribed lifestyle changes and exercise programs to help recover function. Most stroke rehabilitation programs focus on short-term improvement, ending just a few months after a patient has had a stroke. Consequently, over the following years, patients' functional improvement plateaus and their fitness often wanes—a factor that could increase the chance of a second stroke.
"Many stroke survivors believe there's nothing to be gained from further rehabilitation, but our results suggest that health and functional benefits from walking on a treadmill can occur even decades out from stroke," says Macko, professor of neurology at the University of Maryland School of Medicine, noting that one of the patients in the study had significant improvement 20 years after a stroke. "We believe exercise gives individuals a way to fight back against stroke disabilities."
Source: Johns Hopkins Medical Institutions