An innovative approach for implanting a new aortic heart valve without open-heart surgery is being offered to patients at NewYork-Presbyterian Hospital/Columbia University Medical Center. Known as the PARTNER (Placement of AoRTic traNscathetER valves) trial, this Phase 3 multicenter study is being led by national co-principal investigators Dr. Martin Leon and Dr. Craig Smith and is focused on the treatment of patients who are at high risk or not suitable for open-heart valve replacement surgery.
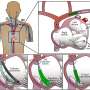
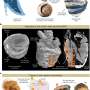
The Edwards SAPIEN transcatheter heart valve, made of bovine pericardial tissue leaflets hand-sewn onto a metal frame, is implanted via one of two catheter-based methods -- either navigated to the heart from the femoral artery in the patient's leg, or through a small incision between the ribs and into the left ventricle. It is then positioned inside the patient's existing valve, using a balloon to deploy the frame, which holds the artificial valve in place. Both procedures are performed on a beating heart, without the need for cardiopulmonary bypass and its associated risks.
"This breakthrough technology could save the lives of thousands of patients with heart valve disease who have no other therapeutic options," says Dr. Leon, the study's national co-principal investigator, associate director of the Cardiovascular Interventional Therapy (CIVT) Program at NewYork-Presbyterian Hospital and Columbia University Medical Center, and professor of medicine at Columbia University College of Physicians and Surgeons.
Annually, some 200,000 people in the U.S. need a new heart valve, but nearly half of them do not receive a new valve for a variety of reasons.
"This study may show that transcatheter valve replacement is a safe and effective alternative to open surgery, which remains the 'gold standard' for most patients," says Dr. Smith, study co-principal investigator, interim surgeon-in-chief and chief of cardiothoracic surgery at NewYork-Presbyterian Hospital/Columbia University Medical Center, and the Calvin F. Barber Professor of Surgery at Columbia University College of Physicians and Surgeons.
The transcatheter valve procedures take about 90 minutes, compared with four to six hours for open-heart surgery. In open-heart surgery, the surgeon cuts through the breastbone, stops the heart, removes the valve and replaces it. Open-heart surgery can require a two- to three-month recovery period, compared to only a few days for the transcatheter approach.
The PARTNER trial is a prospective randomized study with two separate treatment arms. In the surgical arm, patients are randomized to receive either the Edwards SAPIEN transcatheter heart valve or an Edwards surgical valve via open-heart surgery. In the non-surgical, medical management arm, patients considered to be non-operative are randomized to receive either the Edwards SAPIEN transcatheter heart valve or appropriate medical therapy.
Aortic Heart Valve Disease
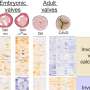
The heart's four valves each have two or three strong tissue flaps, or leaflets, which open and close with each heartbeat, approximately once every second throughout a person's life. When working properly, heart valves ensure that blood flows in the right direction. But when damaged by congenital conditions or progressive disease, these valves can become defective and inhibit efficient blood flow to the body. The aortic valve in particular is prone to age-related stenosis, a narrowing and calcification of the valve opening that, over time, may inhibit adequate oxygenated blood flow to the circulatory system. Aortic valve stenosis may progress for years, with patients experiencing symptoms similar to those associated with aging such as increased fatigue and shortness of breath. As the condition deteriorates, patients also may experience angina (chest pain), light-headedness or fainting. Left untreated, aortic valve disease can ultimately lead to death. More than 5 million Americans have moderate to severe valve disease, where at least one valve does not work properly.
Source: Columbia University Medical Center