(Medical Xpress)—Although some family health innovations have proved effective in communities around the globe, many fail to gain widespread use – particularly in low- and middle-income countries. Researchers at Yale's Global Health Leadership Institute (GHLI) examined several maternal and child health programs—such as those promoting breastfeeding and contraception—and produced an integrated and practical model of how to scale-up such programs.
The study, published in the September issue of BMJ online journal, synthesizes the experiences of family health programs in lower income countries.
"Our findings suggest that successful scale-up occurs within a complex adaptive system, characterized by interdependent parts, multiple feedback loops, and several potential paths to achieve intended outcomes," explains Elizabeth Bradley, faculty director at GHLI and lead author on the paper, titled "A model for scale up of family health innovations in low-income settings: a mixed methods study."
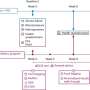
Through a review of the literature and in-depth interviews with various experts, the Yale team developed the AIDED (Assess/Innovate/Develop/Engage/Devolve) model, laying out the five key factors that foster the spread of successful innovations from one community to another.
These factors are:
- Assess the landscape of users' contexts. "Key informants suggested that a primary limitation of scale-up efforts was poor understanding of what communities wanted and what made them receptive to the innovation," write the researchers.
- Innovate to increase user receptivity. The researchers recommended "adapting the innovation to local context and preferences," including "making changes to the design and packaging of the innovation," in order make the program's benefits clearer to potential user groups.
- Develop support for the innovation. "Developing support involved enhancing education as well as identifying and addressing resistance to the innovation," note the researchers, adding, that inadequate development of support and emerging resistance from stakeholders were common reasons cited for failure of scale-up efforts.
- Engage user groups. This is a three-step process, the researchers noted; 1) "introduction," i.e., identifying someone who has "an essential, pre-existing role in the user group" to serve as a "boundary spanner"; 2) "translating," or finding ways to make the innovation understandable and acceptable to potential users, including tapping into local idioms and practices; 3) "integration," which the researchers describe as "the embedding of the innovation in the routines and social norms of a user group."
- Devolve for the spread of innovations. "Relinquishing control over the innovations' spread" is ultimately necessary for full scale-up, noted the researchers, adding that these innovations have to be "reintroduced" to each new potential user group.
Bradley presented the AIDED model last November at the Bill and Melinda Gates Foundation "Achieving Lasting Impact at Scale" convening, which sparked the conversation on impact at scale among researchers, practitioners, policymakers, and funders.
Journal information: British Medical Journal (BMJ)
Provided by Yale University