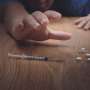
Drug overdose death rates per year in the United States (U.S.) nearly doubled from 1999 to 2013. In New York City (NYC) alone, drug overdose deaths had a 43% increase between 2010 and 2014. The majority of these deaths in NYC involved opioids, with heroin being the most predominant.
A previous survey of 440 drug injectors in NYC conducted in 2015 by the Injection Drug Users Health Alliance found nearly two-thirds (60%) of active injectors surveyed reported using public locations, such as public bathrooms, in the last three months for injections.
"While there are a growing number of syringe exchange programs (SEP) across the U.S. that provide people who inject drugs (PWID) with sterile injecting equipment," said Dr. Brett Wolfson-Stofko, PhD, the lead author and a post-doctoral fellow at the Behavioral Sciences Training in Drug Abuse Research (BST) program at the New York University Rory Meyers College of Nursing (NYU Meyers), "they are not authorized to offer a safe and sanitary space for injection. As a result, many tend to inject in public bathrooms."
Public injection has been associated with a variety of health risks and risk behaviors such as syringe sharing, overdose, abscesses, endocarditis, rushed injection, incarceration, and the transmission of HIV, hepatitis C (HCV), and hepatitis B (HBV).
Dr. Wolfson-Stofko saw an opportunity for research, as a large number of NYC businesses provide public bathrooms. The results of the study were published in the International Journal of Drug Policy and entitled, "Drug Use in Business Bathrooms: An exploratory study of manager encounters in New York City." The study looked at the frequency of business manager encounters with drug use occurring in their business bathroom.
Eighty-six business managers participated in the survey with 58% (50 managers) reporting encounters with drug use in their business bathrooms in the past six months. Data was not used from the 36 managers who did not report encountering drug use.
The research team found that managers reported a median of three encounters with drug use per month. Fourteen percent (7 managers) called 911 due to encounters with unresponsive users. Nearly half of managers who called 911 requested both law enforcement and EMS, suggesting the calls were not solely made because of disruptive behavior, but out of concern for the individual's health. Additionally, over a third of managers found improperly disposed syringes in their business' bathrooms, putting PWID, community members, and staff at risk of needle sticks and potentially HIV, HCV, and HBV infection.
"These managers, by default, are first-responders in the event of a drug overdose and thus of intrinsic interest during the current epidemic of opioid-related overdoses in the U.S." said Dr. Wolfson-Stofko.
The survey found that only 10% of these managers reported some type of overdose recognition and naloxone training. Unsurprisingly, 64% thought this training would be useful and is something Dr. Wolfson-Stofko is currently pursuing.
The researchers also suggest the operation of supervised injection facilities (SIF)/drug consumption rooms (DCR), which are places where people are legally allowed to consume illicit drugs under the supervision of medical staff in order to prevent overdose mortalities, the spread of disease, and reduce the improper disposal of syringes and public injecting.
"Supervised injection facilities and drug consumption rooms are practical, cost-effective strategies that would more than likely reduce public injecting and overdose mortality in New York City and assist in linking this population to health services and drug treatment just as they have in other cities throughout the world," said Dr. Wolfson-Stofko.
"These facilities would also help reduce the burden placed on business managers and staff whose bathrooms act as de facto injection sites," continues Dr. Wolfson-Stofko. "These individuals are not typically trained to handle these types of situations on the job."
The authors argue that implementing multiple SIF/DCR throughout the city would be the best strategy to address public injection and the current overdose epidemic.
In the long term, the researchers hope to help reduce the dangers of public drug injection and improve the overall health of people who use drugs and their communities. Dr. Wolfson-Stofko is expanding upon this research by conducting interviews with staff, managers, and owners of businesses about their perspectives on drug use and overdose as well as well as offering them free naloxone and training through the NDRI opioid overdose prevention program.
More information: Brett Wolfson-Stofko et al. Drug use in business bathrooms: An exploratory study of manager encounters in New York City, International Journal of Drug Policy (2017). DOI: 10.1016/j.drugpo.2016.08.014
Journal information: International Journal of Drug Policy
Provided by New York University