Patients with undiagnosed or untreated obstructive sleep apnea are especially vulnerable to the effects of sleep deprivation and even legal doses of alcohol when it comes to lowered driving performance and increased risk of vehicular accidents, according to new research to be announced on May 19 at the American Thoracic Society's 105th International Conference in San Diego.
Andrew Vakulin, a Ph.D. candidate at the Adelaide Institute for Sleep Health, and colleagues investigated the effects of sleep restriction and moderate alcohol exposure on patients with OSA with respect to their performance on a simulated driving task.
Driver sleepiness is already known to contribute to about one in three car accidents, and OSA patients are known to be at greater risk. However, the extent to which OSA exacerbates the effects of normal sleepiness or alcohol consumption on driving ability was not previously known.
"We found that patients with OSA had a significantly poorer performance than their peers without OSA on the driving task after sleep restriction or alcohol exposure, even though the alcohol dose was clearly within the limits imposed by most state laws—about equal to having two drinks for a woman or three for a man over the course of an hour," said Mr. Vakulin.
Patients with OSA were recruited following a standard diagnostic sleep study at the Adelaide Institute for Sleep Health prior to commencement of treatment. Healthy volunteers were randomly recruited from the community through newspaper advertisements and were matched by age and sex to the patient group. There were a total of 38 OSA patients and 20 healthy individuals tested.
All subjects completed a 90-minute mid-afternoon simulated driving course after normal sleep (about eight hours), sleep restriction (about four hours) and consumption of alcohol (to blood alcohol levels of approximately 0.05g/dL). The road course simulated a country night-time drive on a predominantly straight dual-lane road with bends occurring at 10 minute intervals, each taking approximately 30 seconds to negotiate. There was no oncoming traffic or traffic lights.
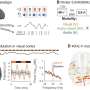
After sleep restriction, individuals with OSA performed significantly more poorly on steering than the 20 healthy individuals. Subjects with OSA were also more likely to crash than control subjects after undergoing both sleep restriction and alcohol exposure.
"While this research could only ethically examine driving performance in a simulated setting, it raises some red flags that have strong real-world implications," said Mr. Vakulin. "In OSA patients, microsleeps [brief episodes of sleep] and prolonged eye closures (greater than two seconds) were significant predictors of having a crash incidents with adjusted odds ratios of 19.2 and 7.2, respectively.
"Clearly this data indicates that people with suspected or untreated sleep apnea should avoid driving if they have not had a full night's sleep, and should avoid driving after consuming even a small amount of alcohol," said Mr. Vakulin.
Source: American Thoracic Society (news : web)