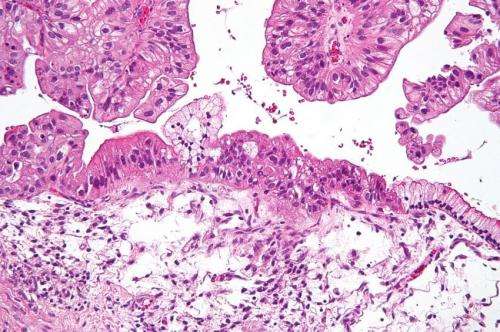
Intermediate magnification micrograph of a low malignant potential (LMP) mucinous ovarian tumour. H&E stain. The micrograph shows: Simple mucinous epithelium (right) and mucinous epithelium that pseudo-stratifies (left - diagnostic of a LMP tumour). Epithelium in a frond-like architecture is seen at the top of image. Credit: Nephron /Wikipedia. CC BY-SA 3.0
One of the largest ever randomised trials has concluded that ovarian cancer screening may reduce ovarian cancer mortality by an estimated 20% after follow up of up to 14 years. Longer follow-up is needed to determine the ultimate mortality reduction and if screening the general population is cost effective.
The United Kingdom Collaborative Trial of Ovarian Cancer Screening (UKCTOCS), published in The Lancet, is led by Professor Ian Jacobs, Institute for Women's Health, University College London, UK, University of University of New South Wales, Sydney, Australia, and University of Manchester, UK; and Professor Usha Menon, Institute for Women's Health, University College London, UK and colleagues. The trial was funded by the UK Medical Research Council, the Department of Health for England, and charities Cancer Research UK and the Eve Appeal.
Professor Jacobs says: "These results from UKCTOCS provide estimates of the mortality reduction attributable to ovarian cancer screening which range from 15% to 28%. Further follow up in UKCTOCS will provide greater confidence about the precise reduction in mortality which is achievable. It is possible that the mortality reduction after follow up for an additional 2-3 years will be greater or less than these initial estimates."
Ovarian cancer continues to be diagnosed at an advanced stage, with 60% of patients dying within five years of diagnosis. UKCTOCS tested the hypothesis that screening for ovarian cancer in the general population can reduce disease mortality without significant harm (in line with screening programmes for other cancers).
Following invitations to 1·2 million women aged 50-74 years identified through age/sex registers, 202 638 were recruited between 2001-2005 to this randomised controlled trial through 13 trial centres in England, Northern Ireland and Wales. Postmenopausal women not considered to be at risk for familial ovarian cancer, with no personal history of ovarian cancer or removal of both ovaries (bilateral oophorectomy) or active non ovarian malignancy were randomised in a 2:1:1 ratio to:
- No screening—101299 women analysed
- Annual screening using serum CA125 (a biomarker blood test) interpreted using the Risk of Ovarian Cancer Algorithm (ROCA) with transvaginal ultrasound scan (TVS) as a second-line test (multimodal; MMS group) - 50624 women analysed or
- Annual TVS alone (USS group)—50623 analysed.
Annual screening ended in December 2011 and follow-up lasted until 31st December 2014. Follow-up was through national cancer/death registries supplemented with postal questionnaires sent to all participants who were alive and had not withdrawn from the study. The primary outcome was death due to ovarian cancer (malignant neoplasm of ovary, fallopian tube or undesignated ovary/tube/peritoneum). An outcome review committee blinded to the randomisation group assigned ovarian cancer diagnosis/death.
The median follow-up was 11·1 years, and ovarian cancers were diagnosed in 630 (no screening) 338 (MMS) 314 (USS) women. The primary analysis using a statistical method known as a Cox model gave a mortality reduction over years 0-14 of 15% with MMS, and 11% with USS which were not significant. This mortality reduction was made up of an 8% and 23% relative reduction in mortality during years 0-7 and 7-14 respectively in the MMS versus no screening analysis; and of 2% and 21% respectively in the USS group.
After excluding women who, when they joined the trial, had undiagnosed ovarian cancer, there was a significant reduction in deaths with an average mortality reduction of 20% and in years 7-14 of 28%. There was also a significant reduction in deaths in the MMS versus no screening group using a different statistical analysis called weighted log rank test. However, this was not a planned analysis and was undertaken only after the data were revealed.
The preliminary estimate of the number needed to screen in the MMS group to prevent one ovarian cancer death at 14 years was 641. In respect to harms, in the MMS group from 10,000 women screened, 14 underwent screen-positive surgery that resulted in benign pathology or normal ovaries, a rate of 2·2 women per screen detected ovarian cancer. In these women, the major complication rate following this surgery was 3·1%.
Professor Menon says: "Our report on the mortality data from UKCTOCS is the first evidence from a randomised controlled trial that screening can reduce ovarian cancer deaths. The findings are of importance given the limited progress in treatment outcomes for ovarian cancer over the last 30 years."
The authors add: "The current relative mortality reduction for the MMS group is estimated at 15%. However, this is made up of little or no reduction (8%) for the first 7 years, with 23% relative mortality reduction between years 7-14. From the analysis excluding prevalent cases, a preliminary estimate of the long-term effect of an MMS screening programme is approximately a 28% mortality reduction after year 7."
UKCTOCS is the largest randomised controlled trial of ovarian cancer screening, and one of the largest individually randomised trials ever performed, with over 202 000 participants and over 2 million women. The authors note the scale of relative reduction in mortality is in keeping with relative reductions in breast cancer randomised screening trials which vary between 15 to 25% with more recent estimates of 13 to 17% in meta-analyses of observational studies. Using UK population data from 2007, a previous study by Loberg and colleagues reported that for every 1,000 women invited to mammography screening every 2 years for 20 years from age 50, 2 to 3 women are prevented from dying of breast cancer.
The authors say "The evidence from UKCTOCS suggests that carefully conducted screening using a multimodal strategy detects ovarian cancer sufficiently early to alter the natural history of the disease and reduce mortality. This opens up a new era in ovarian cancer research and care. Whether or not population screening is justified will depend upon a range of factors including further follow-up to determine the full extent of the mortality reduction and health economic analyses. Meanwhile efforts can be made to refine ovarian cancer screening, develop tests with greater sensitivity and more lead time and improve ways to risk stratify the population."
In a Comment, Professor René Verheijen and Dr Ronald Zweemer, Department of Gynaecological Oncology, UMC Utrecht Cancer Center, Netherlands, say: "If only 59% of ovarian cancer cases are detected by screening plus ultrasound, we will need to focus on why and how screening—as undertaken within UKCTOCS—still has a significant, but delayed, survival effect. Trying to unravel the mechanism behind this effect so that it can be improved should have high priority...Awareness and symptom recognition for diagnosis of cancer at an early stage will be difficult to improve upon. Screening will not be warranted until the UKCTOCS outcome has been validated in daily practice. But careful studies such as that of Jacobs and colleagues show that we must and can focus on mechanisms of early cancer detection."
More information: The Lancet, www.thelancet.com/journals/lan … (15)01224-6/abstract
Journal information: The Lancet
Provided by Lancet