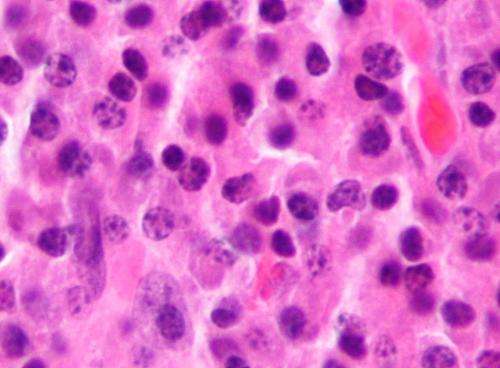
Micrograph of a plasmacytoma, the histologic correlate of multiple myeloma. H&E stain. Credit: Wikipedia/CC BY-SA 3.0
The addition of bortezomib to a standard two-drug regimen for multiple myeloma patients significantly lengthened the time before their cancer returned, and significantly lengthened their lives, according to clinical trial results in The Lancet.
Investigators from SWOG, the international cancer clinical trials network funded by the National Cancer Institute (NCI), compared the effectiveness of two drug regimens in newly diagnosed patients undergoing their first round of treatment for multiple myeloma, a type of bone marrow cancer. One regimen used in the study was lenalidomide with dexamethasone, a standard first-line treatment. The other drug regimen also included bortezomib, a second-line drug typically given to myeloma patients whose cancer progresses after initial therapy.
SWOG researchers found that the addition of bortezomib made a significant difference for myeloma patients, giving them about another year of remission and another year of life.
Patients receiving bortezomib, along with lenalidomide and dexamethasone, in their first six months of treatment had a median remission time of 43 months compared to a median remission of 30 months for patients who received lenalidomide and dexamethasone alone. Researchers also found that patients who received bortezomib lived a median of 75 months, or about six years, after their initial treatment. Patients who received the standard two-drug treatment lived a median of 64 months, or about five years, after initial treatment.
"There's a lot of excitement about these research findings and this treatment option, which helps myeloma patients stay healthier longer and gives them more time to spend with people they love," said SWOG study principal investigator Brian G.M. Durie, M.D., a physician at Cedars-Sinai Outpatient Cancer Center in Los Angeles and chairman of the board at the International Myeloma Foundation. "Because the research was so solid, and the findings so strong, we're looking at a potential new standard of care."
Results of the SWOG study, S0777, first gained attention in December 2015 at the 57th Annual Meeting of the American Society of Hematology (ASH) held in Orlando, Florida. Myeloma is the second most common blood cancer in the world. According to NCI statistics, in 2016 an estimated 30,330 new cases of myeloma will be diagnosed and 12,650 people will die of the disease in the U.S. In recent years, new drugs have brought new hope, and life expectancy for people diagnosed with multiple myeloma is slowly rising.
SWOG researchers enrolled 471 eligible and consented adult patients in S0777 between February 2008 and February 2012 at 139 institutions throughout the National Cancer Trials Network (NCTN), the nation's oldest and largest publicly funded cancer research network. The NCTN includes SWOG, the Alliance for Clinical Trials in Oncology, ECOG-ACRIN Cancer Research Group, and NRG Oncology, which all enrolled patients to S0777, as well as the Children's Oncology Group, which focuses on pediatric cancers.
S0777 patients ranged in age from 28 to 87, had active myeloma, and had not had a stem-cell transplant or any prior treatment for their disease. Patients were randomized into two groups. One group received the standard two-drug treatment for six cycles over six months. That includes lenalidomide, an immunomodulating therapy marketed as Revlimid by Celegene Corporation. The other group received a three-drug combination that included bortezomib, a proteasome inhibitor marketed as Velcade by Millennium Pharmaceuticals. These patients received the triple combination therapy for eight cycles over six months.
Despite the increased remission and longevity, the three-drug combination did have a drawback: Patients who received bortezomib were much more likely to experience sensory neuropathy, or tingling, pain, numbness or weakness in their hands and feet.
Journal information: The Lancet
Provided by SWOG