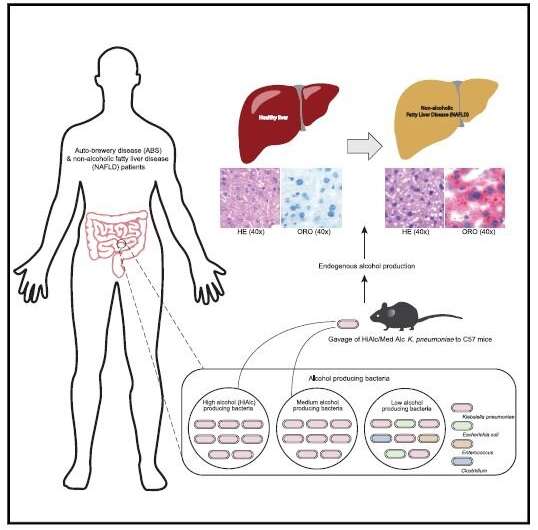
This graphical abstract shows how high-alcohol-producing Klebsiella pneumoniae (HiAlc Kpn) occurs in a large percentage of individuals with nonalcoholic fatty liver disease (NAFLD). Credit: Yuan et al./Cell Metabolism
Non-alcoholic fatty liver disease (NAFLD) is the build-up of fat in the liver due to factors other than alcohol. It affects about a quarter of the adult population globally, but its cause remains unknown. Now, researchers have linked NAFLD to gut bacteria that produce a large amount of alcohol in the body, finding these bacteria in over 60% of non-alcoholic fatty liver patients. Their findings, publishing September 19 in the journal Cell Metabolism, could help develop a screening method for early diagnosis and treatment of non-alcoholic fatty liver.
"We were surprised that bacteria can produce so much alcohol," says lead author Jing Yuan at Capital Institute of Pediatrics. "When the body is overloaded and can't break down the alcohol produced by these bacteria, you can develop fatty liver disease even if you don't drink."
Yuan and her team discovered the link between gut bacteria and NAFLD when they encountered a patient with severe liver damage and a rare condition called auto-brewery syndrome (ABS). Patients with ABS would become drunk after eating alcohol-free and high-sugar food. The condition has been associated with yeast infection, which can produce alcohol in the gut and lead to intoxication.
"We initially thought it was because of the yeast, but the test result for this patient was negative," Yuan says. "Anti-yeast medicine also didn't work, so we suspected [his disease] might be caused by something else."
By analyzing the patient's feces, the team found he had several strains of the bacteria Klebsiella pneumonia in his gut that produced high levels of alcohol. K. pneumonia is a common type of commensal gut bacteria. Yet, the strains isolated from the patient's gut can generate about four to six times more alcohol than strains found in healthy people.
Moreover, the team sampled the gut microbiota from 43 NAFLD patients and 48 healthy people. They found about 60% of NAFLD patients had high- and medium-alcohol-producing K. pneumonia in their gut, while only 6% of healthy controls carry these strains.
To investigate if K. pneumonia would cause fatty liver, researchers fed germ-free mice with high-alcohol-producing K. pneumonia isolated from the ABS patient for 3 months. These mice started to develop fatty liver after the first month. By 2 months, their livers showed signs of scarring, which means long-term liver damage had been made. The progression of liver disease in these mice was comparable to that of mice fed with alcohol. When the team gave bacteria-fed mice with an antibiotic that killed K. pneumonia, their condition was reversed.
"NAFLD is a heterogenous disease and may have many causes," Yuan says. "Our study shows K. pneumonia is very likely to be one of them. These bacteria damage your liver just like alcohol, except you don't have a choice."
However, it remains unknown why some people have high-alcohol-producing K. pneumonia strain in their gut while others don't.
"It's likely that these particular bacteria enter people's body via some carriers from the environment, like food," says co-author Di Liu at the Chinese Academy of Sciences. "But I don't think the carriers are prevalent—otherwise we would expect much higher rate of NAFLD. Also, some people may have a gut environment that's more suitable for the growth and colonization of K. pneumonia than others because of their genetics. We don't understand what factors would make someone more susceptible to these particular K. pneumonia, and that's what we want to find out next."
This finding could also help diagnose and treat bacteria-related NAFLD, Yuan says. Because K. pneumonia produce alcohol using sugar, patients who carry these bacteria would have a detectable amount of alcohol in their blood after drinking a simple glucose solution. "In the early stages, fatty liver disease is reversible. If we can identify the cause sooner, we could treat and even prevent liver damage."
"Having these bacteria in your gut means your body is exposed to alcohol constantly," Liu says. "So does being a carrier mean you would have higher alcohol tolerance? I'm genuinely curious!"
More information: Cell Metabolism, Yuan et al.: "Fatty liver disease caused by high alcohol-producing Klebsiella pneumoniae" www.cell.com/cell-metabolism/f … 1550-4131(19)30447-4, DOI: 10.1016/j.cmet.2019.08.018
Journal information: Cell Metabolism
Provided by Cell Press