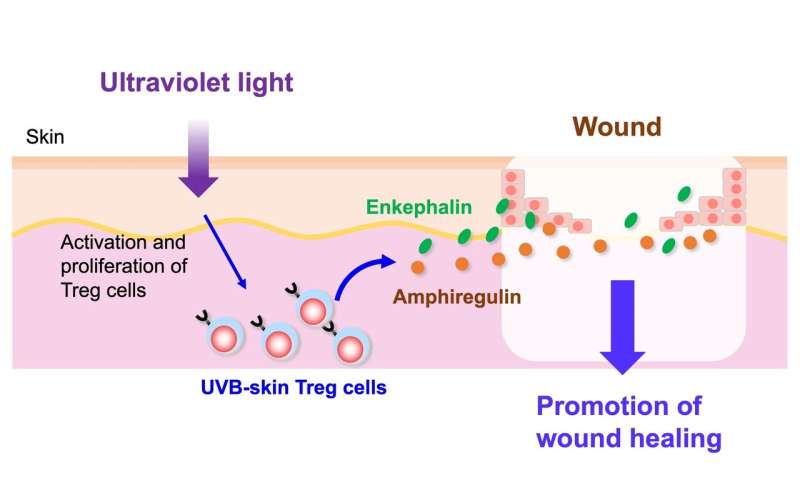
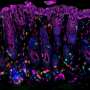
UVB irradiation induces proliferation and activation of skin Treg cells. UVB-expanded skin Treg (UVB-skin Treg) cells promote wound healing by producing enkephalin and amphiregulin(AREG), which enhance keratinocyte growth/proliferation to repair skin wound. Credit: Department Immunology, Nagoya City University Graduate School of Medical Sciences
Ultraviolet B (UVB) is used as an effective therapy for individuals with psoriasis and atopic dermatitis because it has an immunosuppressive effect. The immune system develops to protect the body from infection or cancer. Its activation affects many physiological functions. Regulatory T (Treg) cells, expressing CD25 and Foxp3, constitute about 5-10% of peripheral CD4+T cells and work as brake on the immune system through the suppression of various immune responses.
Researchers from Nagoya City University previously showed that skin Treg cells were expanded by UVB up to about 60% of CD4+T cells.
Here they found that UVB-expanded skin Treg (UVB-skin Treg) cells had a healing function. UVB-skin Treg cells expressed proenkephalin (PENK), an endogenous opioid precursor, and amphiregulin (AREG), the epidermal growth factor receptor ligand, which promoted wound healing in vivo and keratinocyte outgrowth in a skin explant assay.
Their results provide a new implication in developing a novel therapy using PENK+UVB-skin Treg cells.
More information: Hiroaki Shime et al, Proenkephalin+regulatory T cells expanded by ultraviolet B exposure maintain skin homeostasis with a healing function, Proceedings of the National Academy of Sciences (2020). DOI: 10.1073/pnas.2000372117
Journal information: Proceedings of the National Academy of Sciences
Provided by Nagoya City University