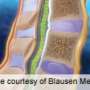
Symptoms from lumbar spinal stenosis, an anatomical impairment common with aging, were relieved and function improved in as many patients utilizing physical therapy as those taking the surgical route, University of Pittsburgh researchers discovered in a two-year study published today in Annals of Internal Medicine.
It is the first study that clearly compared outcomes between surgery and an evidence-based, standardized physical therapy approach for lumbar spinal stenosis. The condition, created by a narrowing of the spinal canal that puts pressure on the nerve roots resulting in pain, numbness and weakness through the back and lower extremities, has caused decompression surgery to become the fastest-growing intervention in today's older population.
A total of 169 patients aged 50-plus already headed for decompression surgery agreed to be randomly assigned into two groups: Those who would have the procedure, and those who went through two standardized, evidence-based physical therapy sessions per week for six weeks. After both groups were re-examined at intervals of six months, one year and two years, the patient outcomes appeared to be equal. There were no detectable differences between the groups in how their pain abated and the degree to which function was restored in their backs, buttocks and legs.
"Probably the biggest point to put across to physicians, patients and practitioners is: Patients don't exhaust all of their non-surgical options before they consent to surgery. And physical therapy is one of their non-surgical options," said principal investigator Anthony Delitto, Ph.D., chair of the Department of Physical Therapy, Pitt School of Health and Rehabilitation Sciences (SHRS), as well as a member of Pitt's Health Policy Institute (HPI) and a consultant to UPMC.
Dr. Delitto, a physical therapist, and his SHRS colleagues have long puzzled over why some patients reacted well to physical therapy (PT) and others to surgery.
"The idea we had was to really test the two approaches head to head," he said. "Both groups improved, and they improved to the same degree. Now, embedded in that, there are patients who did well in surgery, and patients who failed in surgery. There are patients who did well in PT, and there are patients who failed with PT. But when we looked across the board at all of those groups, their success and failure rates were about the same."
The research project also revealed issues surrounding PT appointments and the cost of co-pay, which may prove enlightening to policymakers enmeshed in the charged atmosphere around health care, Dr. Delitto added.
Most patients didn't finish the PT regimen allowed them under Medicare and prescribed by the researchers, and one-third of the patients failed to complete even half of the regimen. Another 16 percent didn't show for a single treatment, though they had agreed to consider PT.
"One of the big things that we know held patients back from PT were co-payments," Dr. Delitto added. "Patients were on Medicare, and a lot of them were on fixed incomes. Some of those co-payments had to come out of pocket at $25, $30, $35 per visit. That adds up, and some of the patients just couldn't afford it."
Journal information: Annals of Internal Medicine