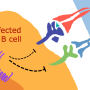
Scientists have identified components of HHV-6 that can be attacked by killer T cells. Credit: Helmholtz Zentrum München
Human herpesvirus 6 infects most people all over the world. It is usually well controlled by the body, but it can cause diseases in immunocompromised individuals. As reported in PLOS Pathogens, scientists at Helmholtz Zentrum München, member in the German Center for Infection Research (DZIF), have now identified virus structures that can be attacked by killer T cells – a possible approach for new therapies.
Most people acquire human herpesvirus 6, or HHV-6 for short, in early childhood. It is a distant relative of the herpes simplex virus known for causing blisters, but HHV-6 has entirely different effects: The infection can lead to a disease called three-day fever in infants and young children. Later, the virus stays in the body and is never eliminated. Although HHV-6 does not affect the health of most people, it is suspected to contribute to autoimmune diseases and chronic fatigue syndrome. One thing is certain: patients with severely weakened immune systems, for example post-transplantation patients, have difficulty keeping the virus under control, which in some cases can result in serious damage to multiple organs.
To counter this risk, scientists at Helmholtz Zentrum München are investigating how the immune system keeps the virus in check. "We are studying the toolbox of the immune system," says Dr. Andreas Moosmann, head of the HOCOVLAR Research Group within the Research Unit Gene Vectors. "Now, we've discovered several interesting new tools that we've already been able to recreate in the lab."
Killer T cells recognize 16 different virus structures
Specifically, the researchers set out to identify those components of the virus that could serve as targets for CD8-positive cells, also known as killer T cells. These cells are capable of destroying infected cells, thus preventing the virus from multiplying in the body.
Led by first author Larissa Martin and doctoral student Alexandra Hollaus, the researchers discovered 16 structures of the virus that HHV-6-specific killer cells can bind and attack. To this end, the scientists first scanned the pathogen with the help of an algorithm that identified nearly 300 potential attack sites. Further analysis narrowed those candidates down to 77 sites. The scientists then succeeded in producing T cells directed against 20 of them, 16 of which actually latched onto their target and destroyed the infected cell.
"We were able to show that very dissimilar proteins of the virus can serve as such attack structures," Andreas Moosmann explains. "We also observed that T cells directed against those structures commonly occur in healthy individuals as well as in transplant patients who control their infection.—Right now, we're verifying this in a large group of patients," adds Dr. Johanna Tischer, stem cell transplantation specialist at Klinikum Grosshadern. In the long term, Andreas Moosmann and his team want to apply their findings to new treatments. "It might be possible to prevent a breakout of the virus by administering HHV-6-specific killer T cells to patients. But before that can be done, we still have a lot of work ahead of us."
More information: Larissa K. Martin et al. Cross-sectional analysis of CD8 T cell immunity to human herpesvirus 6B, PLOS Pathogens (2018). DOI: 10.1371/journal.ppat.1006991
Journal information: PLoS Pathogens
Provided by Helmholtz Association of German Research Centres