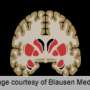
A study co-led by Dr. Nelly Mauras at Nemours Children's Health System in Jacksonville, Florida found that children with type 1 diabetes (T1D) have slower growth in brain areas associated with mild cognitive deficits compared to children without T1D. The study, presented today at the American Diabetes Association's (ADA's) 79th Scientific Sessions, found significant differences in total brain and regional gray and white matter growth based on a series of three structural magnetic resonance imaging (MRI) studies.
"Even with new insulin and technologies that can significantly improve care, children with Type 1 Diabetes are still exposed to significant swings in sugar control, creating potential risks to the developing brain," said Nelly Mauras, MD, co-principal investigator of the study, chief of the division of endocrinology, diabetes & metabolism at the Nemours Children's Health System in Jacksonville, Florida, and professor of pediatrics at the Mayo College of Medicine. "Understanding the early effects of blood sugar control on brain development is a necessary step towards developing strategies for reducing these risks and the public health implications of diabetes-related cognitive dysfunction later on in life."
As part of a multi-site study of the Diabetes Research in Children Network (DirecNet), researchers aimed to determine the extent to which glycemic exposure adversely impacts the developing brain in children with early-onset T1D. The study enrolled 138 children with T1D with a median age of seven years. The participants had a disease duration on average of 2.4 years at the beginning of the study. MRIs were performed at three time points (baseline visit, 18 months and approximately 2.9 years after the second visit) to measure gray and white matter volumes in key brain regions. Total cumulative hyperglycemic exposure was determined using lifetime blood sugar, using hemoglobin A1c (HbA1c) values from the time of diagnosis. Researchers compared the MRI results of T1D participants to those of a control group of 66 age-matched children who did not have diabetes.
Researchers found that the group with T1D had slower growth of total cortical and subcortical gray and white matter than the control group at all time points. In particular, a set of metabolically active brain regions associated with other brain disorders, known as the "default mode network," showed less growth in the T1D group compared to the control group. These regions of slower growth were associated with higher lifetime blood sugar, as measured by HbA1c values.
"Ongoing research is investigating whether diligent maintenance of blood sugar levels in the normal range through advanced diabetes technologies can impact these findings to reduce the risk for cognitive dysfunction," said Mauras.
Provided by Nemours Children's Health System