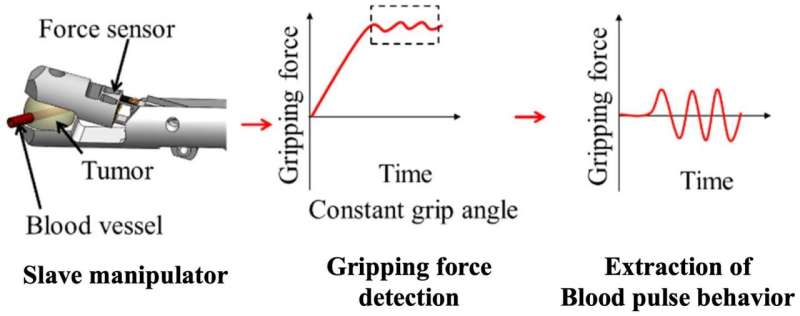
Blood pulse detection at a constant gripping angle. As a basic test, a gripper with force sensor held the tumor with blood vessel at a constant grip angle. Then blood pulse is detected as the vibration of the gripping force. Credit: Kanazawa University
During neuroendoscopic surgery of, for example, brain tumors, the characteristics of the operating space, usually narrower than that of other endoscopic surgeries, are determined by visual inspection through the endoscope. However, when bleeding occurs, the surgical site is covered in blood, disrupting visualization. The surgeon may intend to resect a tumor with minimal hemorrhage but can unintentionally cut a blood vessel in the tumor that could not be confirmed visually. Therefore, identification of the presence of blood vessels during brain tumor resection is critical. So far, a number of studies have developed methods to detect invisible blood vessels. Nonetheless, further development of such methods is crucial.
In laparoscopic surgery, blood vessels can be detected using a force/tactile feedback system. However, in neurosurgery, it is difficult to detect blood vessels using the existing force/tactile feedback method because the thickness of the target blood vessels is different from that in laparoscopic surgery. In addition, during brain tumor resection under a neuroendoscope, the surgical site is often covered in blood even with minor bleeding since the operating space is very narrow.
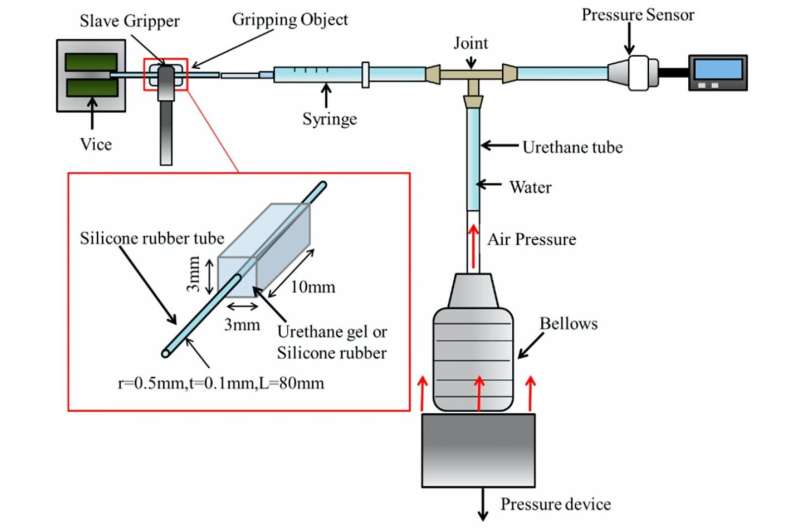
Schematic view of the present experimental equipment. Blood vessel detection system was developed using a silicone rubber tube as a blood vessel and urethane gel or silicone rubber as tumor. Blood vessel pulsation is applied by cyclic water pressure vibration from bellows type pressure device and pressure is detected by pressure sensor. Credit: Kanazawa University
Scientists in the fields of mechanical engineering and medicine at Kanazawa University have collaborated to develop a method for detecting blood vessels inside tumors that are otherwise visually undetectable. They previously developed a surgical robot manipulator with a force feedback system and demonstrated the benefits of the system in neurosurgery. However, detection of blood vessels using the existing force/tactile feedback system is difficult in neurosurgery as described above.
In this study, they developed a novel blood vessel detection method that uses a master-slave surgical robot system with a force sensor at the operating segment. The method detects blood pulsation based on gripping force.
If there is a thin artery in a tumor, pulsation of such an artery should be detected by applying an appropriate force sensor to the gripper. However, since the hardness of tumors varies to a considerable extent, such a pulsation sensing system should be applicable to both soft tumors and hard tumors. In addition, since arterial pulsation is much smaller than the tumor-gripping force, such sensor systems must be able to detect even small force changes while gripping a tumor and to have an adequate response time for detecting pulsation.
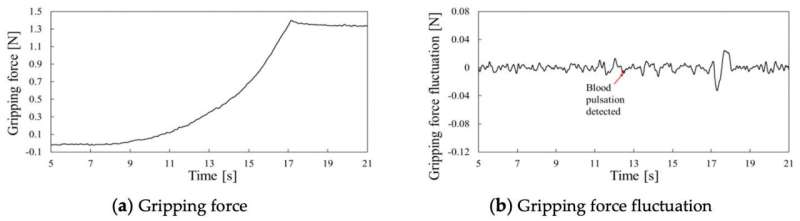
Gripping force behavior with a simulated tumor of silicone rubber at a gripping speed of 2.5°/s. Detection test of the blood pulsation in the period of gripping process. During the closing of the gripper, gripping force increases as shown in Figure 3 (a). In the process of increasing gripping force, pulsation of the blood vessel appears as cyclic force fluctuation as shown in Figure 3(b). Credit: Kanazawa University
In this study, a gripper of 3 mm diameter has been developed as shown in Figure 1 left. The force sensor integrated in the gripper detects and records pulsation of an artery in a tumor and the gripping force when the gripper grips a tumor. Since human pulsation is about 70 per minute, the time interval of force measurement was set to 5 msec. As seen in the second panel from the left of Figure 1, pulsation was detected and its frequency could be measured.
A simulated soft or hard tumor was made from urethane gel with 10% added salt or from silicone rubber. The dimension of a simulated tumor was 3 × 3 × 10 mm, and at the center along the long axis, silicone rubber tubing (radius = 0.5 mm and thickness = 0.1 mm) was inserted as a simulated artery. The Young's moduli of urethane gel and silicone rubber, measured in a preliminary experiment, were 6 and 38 kPa, respectively. In a study of fluid analysis in cerebral aneurysm, the Young's modulus of a normal blood vessel wall in the brain was found to be 1 MPa, while that of the silicone rubber tube measured in a preliminary experiment was 1.9 MPa. Water was passed through this model artery with a pulsation of 1.2 Hz to simulate blood flow.
The gripper with an opening angle of 34° was designated to be 0° and the closing speed was adjusted. One of the results with urethane gel is shown in Figure 2. With urethane gel, a simulated soft tumor, pulsation was detected at 30° (4° aperture). On the other hand, with silicone rubber as a simulated hard tumor, pulsation was detected at 15-25° (9-19° aperture).
Thus, the scientists were successful in detecting pulsation of a simulated brain artery of 1 mm diameter in simulated soft and hard tumors. Although they present only basic results on the detection of the blood pulses inside simulated tumors during the gripping process, they believe that this new system will be useful for surgeons. If the surgeon suspects the existence of blood vessels inside a tumor, then gripping the tumor can be prolonged to determine blood pulses in the gripping force wave of the manipulator. Although the detection accuracy and speed of this method needs to be improved, it should be effective in avoiding hemorrhage during tumor resection, thus providing a route for tumor resection.
More information: Hiroki Yokota et al, Method for the Detection of Tumor Blood Vessels in Neurosurgery Using a Gripping Force Feedback System, Sensors (2019). DOI: 10.3390/s19235157
Provided by Kanazawa University