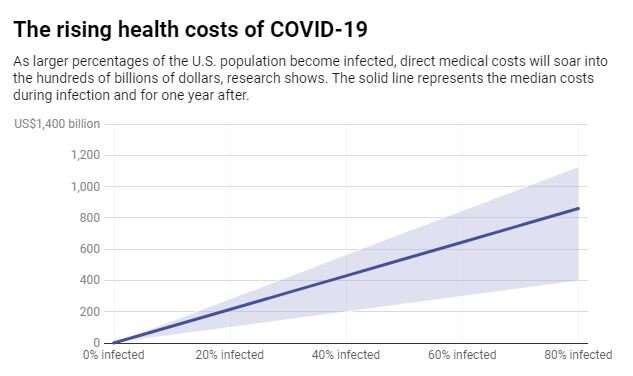
The lower bound represents a scenario in which key parameters seen in medical care today decline, specifically reductions in the probabilities of severe disease requiring hospitalization by 50%, ICU admission by 20%, and death by 95%. The upper bound represents a scenario in which key parameters rise, including increasing the probabilities of hospitalization and ICU admission by 20%. Credit: Chart: The Conversation, CC-BY-ND Source: Bartsch, et al, Health Affairs
As states push to reopen businesses, arguing their economies are losing too much money under current coronavirus precautions, they can't ignore the other side of the economic equation—the one involving human lives and potentially hundreds of billions of dollars in medical costs.
More than 20,000 new COVID-19 cases are still being reported in the U.S. every day, and the coronavirus that causes it is still spreading.
If the U.S. reopens its economy prematurely and COVID-19 cases surge again, medical expenses will surge, too. Someone has to pay those costs. If you own a business, pay for health insurance or pay taxes, that someone is you.
To get a better sense of what the nation's COVID-19-related health care costs could be as more and more of the population is infected, our Public Health Informatics, Computational, and Operations Research team at the City University of New York (CUNY) Graduate School of Public Health and Health Policy developed a computer simulation of the entire United States.
It allows us to quantify what could happen depending on how the pandemic progresses and the resulting direct medical costs and health care resource needs. The results were published in the journal Health Affairs.
Building a Sim nation for COVID-19
Our team develops computer simulation models to help decision-makers better understand and address different infectious diseases, including MRSA, the flu, Zika and Ebola. During the 2009 H1N1 influenza pandemic, the team was embedded in the U.S. Department of Health and Human Services to help with the national response.
These models try to recreate all of the people, processes, resources and systems involved in a given health or public issue, such as a pandemic, to serve as virtual worlds to test different possible scenarios, policies and interventions and calculate the expected costs.
For this latest coronavirus model, we created virtual representations of the entire U.S. population.
Each virtual person had probabilities of becoming infected with the new coronavirus, SARS-CoV-2. Like a real person, the virtual person had chances of developing mild or severe symptoms, or having no symptoms at all during the course of the infection. No symptoms naturally meant no health costs.
How medical costs pile up
If the person developed symptoms, what happened next depended on how severe the symptoms became and what the person ended up doing.
For example, treating a child with only a mild illness requiring no more than a telephone call to a doctor would typically cost around US$32 (in most cases ranging from $19 to $56). The cost for an adult in the same situation would be about $17 (in most cases ranging from $16 to $67). Our model incorporated the variations in costs that occur, so that two people could have the exact same paths, yet still have different costs.
Not surprisingly, costs increased substantially if the person had more severe symptoms that required hospitalization.
The costs of a hospital bed, health care personnel, medications and potentially the use of medical equipment such as ventilators quickly add up, pushing up the median cost for a person hospitalized to $14,366.
Most COVID-19 patients don't require hospitalization, so the median cost for any person with symptoms turned out to be $3,045 during the course of the person's infection. But this is still over four times the typical cost of a symptomatic influenza case and around 5.5 times that of a symptomatic pertussis case. Consider this further evidence that COVID-19 is definitely not "just like the flu."
Health care costs for the coronavirus don't end when the patient leaves the hospital. Patients with severe illness may require follow-up visits to the doctor, imaging such as X-rays and CT scans, lab tests, medications or even additional hospitalizations. Those with significant lung damage, for example, may be more susceptible to subsequent infections.
The resulting health care costs over the year after the initial infection raise this median cost per patient by 30% to $3,994.
This shows that you can't ignore what happens after the initial infection. That would be like walking out of a three-hour movie after just the second hour.
For some patients, the suffering and medical costs don't end once the virus is no longer present. For example, those who experience lung damage may continue to have breathing problems. Those who managed to survive sepsis and organ failure can have a variety of persistent symptoms. Given these persistent problems, for some, COVID-19 may become more like a chronic condition.
Herd immunity and the high cost of viral spread
Our findings also shed light on what can happen when more and more of the population becomes infected.
We found that if 20% of the U.S. population gets COVID-19, it would mean about 11.2 million people would be hospitalized, and the sickest among them would spend a combined 13 million days on ventilators.
This would cost about $163.4 billion in direct medical expenses, and that's before accounting for the costs incurred after the infection is over. It also does not include many other health-related costs, such as physician fees that can vary from doctor to doctor, the costs of public health measures such as widespread testing and the costs of protecting health care workers and other patients.
If half the population becomes infected before a vaccine is ready, the numbers jump to 27.9 million hospitalizations and 32.6 million ventilator days. The median cost: $408.8 billion, rising to $536.7 billion with a year of follow-up medical costs taken into account.
That's getting close to what's known as herd immunity, the point where enough people are immune that the disease no longer finds hosts to spread it. With the coronavirus, herd immunity is believed to be reach when at least 60% of the population has either been infected naturally or vaccinated.
If 80% of the population gets infected, the numbers rise to 44.6 million hospitalizations, 52.2 million ventilator days and $654 billion in direct medical expenses. With a year of follow-up medical expenses included, that median cost rises to $1.25 trillion.
All of this shows what could happen if the country allows more people to become infected by prematurely relaxing social distancing or trying "herd immunity strategies" that just allow people to get infected. The costs also go well beyond health care expenses when lives are at stake.
Good decision-making during this pandemic requires good science and data. Ultimately, not considering the potential associated medical costs can be like ignoring a large part of the field in a football game. And that could be a losing proposition.
Journal information: Health Affairs
Provided by The Conversation
This article is republished from The Conversation under a Creative Commons license. Read the original article.![]()