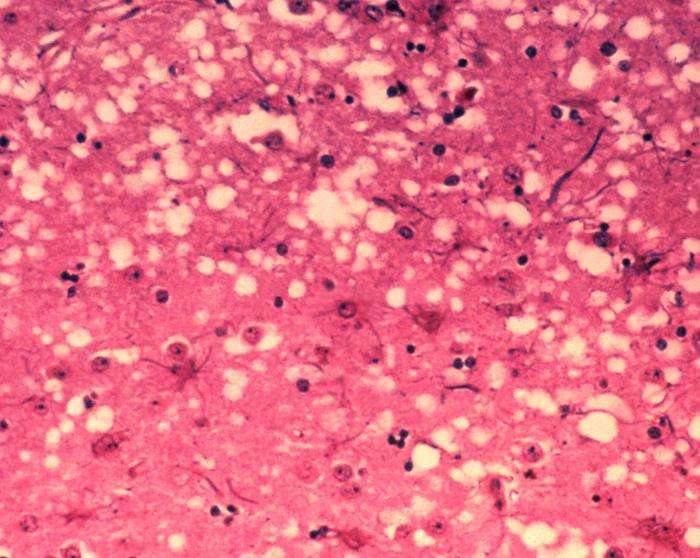
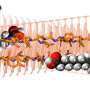
This micrograph of brain tissue reveals the cytoarchitectural histopathologic changes found in bovine spongiform encephalopathy. The presence of vacuoles, i.e. microscopic “holes” in the gray matter, gives the brain of BSE-affected cows a sponge-like appearance when tissue sections are examined in the lab. Credit: Dr. Al Jenny - Public Health Image Library, APHIS: Public domain
Antibodies targeting the normal PrP version of the prion protein have been found in humans selected at random with no history of any associated transmissible spongiform encephalopathies. The significance is that prion proteins can be converted into a disease-causing infectious particle like PrPSc, an aggregated version or isoform resistant to degradation by protease enzymes. Resulting prion diseases, like other neurodegenerative syndromes such as Alzheimer's disease and Parkinson's disease, are associated with accumulation of misfolded and aggregated proteins in the central nervous system. Antibodies against such proteins may be beneficial and offer potential for therapies against such diseases by targeting the pathological aggregates for degradation by phagocytic cells.
Today in EMBO Molecular Medicine, researchers at the University of Zurich and Novartis Institutes for BioMedical Research in Switzerland report on active antibodies against PrP at high levels in a small proportion of individuals, 21 of 37,894 hospital patients screened for presence of anti-PrP IgGs, the most common form of immunoglobulin. There was strong evidence from lack of any past history of disease among these individuals that these antibodies were not themselves neurotoxic. That, combined with the lack of such antibodies among people who do carry disease-causing mutations in the PRNP gene coding for prion proteins, suggests they might have cleared unwanted nascent disease prions early in life.
Earlier research had already shown that anti-PrP antibodies are effective in mice infected with prions and also some human cells, suggesting they might represent a viable therapeutic strategy. However, it has also been demonstrated that the biological effect of anti-PrP antibodies depends critically on which part, or epitope, of the PrP prion recognized by the immune system is targeted. Therefore, the latest work sought to produce a high-resolution map of neuroprotective epitopes, with the ultimate goal of identifying immunotherapeutics that might be effective, as well as safe by avoiding neurotoxic effects. This was achieved by discovering antibodies that targeted both the main globular domain (GD) of the prion protein and its flexible tail (FT). This suggested there was a polyclonal antibody response, offering further evidence for the existence of naturally occurring antibodies against the prion protein in humans.
The resulting immune response capable of clearing nascent infectious prions may then operate analogously to immune surveillance for neoplastic cells that cause cancer. At the very least, generation of antibodies to the whole set of PrP epitopes provides new tools for studying the mechanism of neurodegeneration conveyed by prions.
More information: Assunta Senatore et al. Protective anti‐prion antibodies in human immunoglobulin repertoires, EMBO Molecular Medicine (2020). DOI: 10.15252/emmm.202012739
Journal information: EMBO Molecular Medicine
Provided by European Molecular Biology Organization