Credit: Pixabay
Actively testing large groups of people at increased risk of severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) could be a component of Canada's strategy to get people safely back to school and work, finds new research published in the Canadian Medical Association Journal.
"As workplaces and schools reopen after the first wave of COVID-19 in Canada, testing priorities and strategies are needed to prevent surges in community transmission of SARS-CoV-2," write Dr. Dick Menzies and Dr. Jonathon Campbell, Research Institute of the McGill University Health Center, Montreal, Quebec, with coauthors.
Researchers calculated the costs, staffing needs and laboratory capacity required for systematic testing of five groups:
- Household and non-household contacts of people newly diagnosed with SARS-CoV-2 infection
- All employees of acute care hospitals
- All community health care workers and employees and residents of long-term care facilities
- All employees of essential businesses with major interpersonal or public contact
- All students and employees in elementary and high schools
The authors estimate that one round of universal testing of these at-risk populations would cost $1.3 billion.
"Even if repeated, these costs represent a small fraction of the $169.2 billion in Canadian federal fiscal response to the COVID-19 pandemic as of June 2020," they suggest.
The benefit of widespread testing would be detection and isolation of asymptomatic people infected with SARS-CoV-2. This could prevent community transmission, which otherwise could result in a second wave and a second shutdown.
"Actively testing those at increased risk of acquiring SARS-CoV-2—and isolating individuals found to be infected—could be equally effective to arrest community transmission and is associated with far less social and economic cost," the authors write.
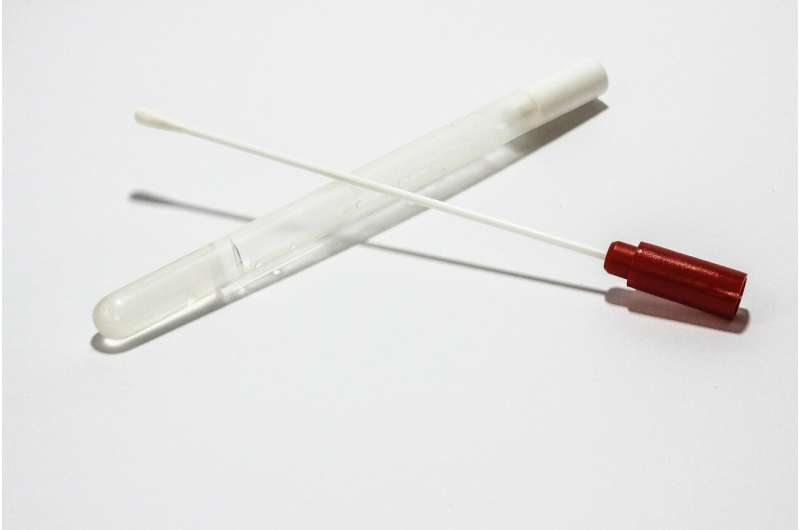
Enlisting other health care professionals, medical students and partnering with academic and private laboratories could help build the capacity required to test on a massive scale, while using saliva-based sampling—as opposed to nasopharyngeal swabs—would cut costs and the number of trained health care professionals needed.
"We believe that a strategy of actively testing large population groups who are at increased risk of acquiring SARS-CoV-2 is feasible and affordable in Canada. This testing approach should be an integral component of a broad strategy to allow all Canadians to return safely to work and school," the authors conclude.
A related CMAJ editorial focuses on the tracing and testing of close contacts of people with SARS-CoV-2.
"Rapid diagnosis and isolation of people with SARS-CoV-2 infection—whether they have symptoms or not—and aggressive tracing, testing and isolation of their contacts, are key to ensuring safety in Canada's school, work and social environments," writes Dr. Andreas Laupacis, editor-in-chief, CMAJ, with coauthors Drs. Larissa Matukas and Irfan Dhalla. "It's time for our governments to fully invest in 'find, test, trace and isolate.'"
The editorial also calls for support of people who may have difficulty self-isolating because of a need to earn income, crowded living conditions or their roles as caregivers.
"Governments must ensure that employees who test positive for SARS-CoV-2 infection continue to be paid while isolating, that facilities such as dedicated hotels are freely and easily available to individuals who cannot self-isolate where they live, and that additional supports—such as help obtaining groceries—are readily obtainable," urge the authors.
The editorial calls for public reporting of the number of close contacts who are identified each day, the number of contacts tested and successfully quarantined, and the time from sample collection to the result becoming available, which they suggest should be less than 24 hours.
More information: Larissa M. Matukas et al. Aggressively find, test, trace and isolate to beat COVID-19, Canadian Medical Association Journal (2020). DOI: 10.1503/cmaj.202120
Journal information: Canadian Medical Association Journal
Provided by McGill University