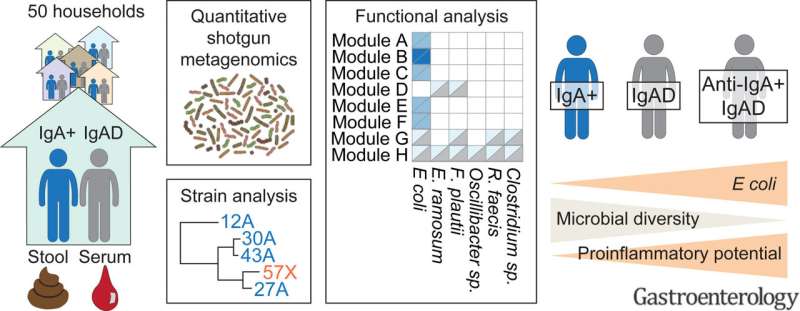
Graphical abstract. Credit: DOI: 10.1053/j.gastro.2021.02.053
In the largest study of intestinal bacterial composition (also called the intestinal microbiome) to date in persons with the immunodeficiency selective IgA deficiency, researchers at DTU Bioengineering have ascertained that people with IgA deficiency have a much more frequent incidence of E. coli, and that there are several intestinal factors that have a correlation with inflammatory and pathogenic processes.
Selective IgA deficiency is one of the most common immunodeficiencies and it occurs in approximately 1 in 600 in Denmark. Persons with IgA deficiency lack a specific antibody—immunoglobulin A—which is otherwise found in all the mucous membranes of the body, where it binds to microorganisms and thus helps protect against infections from pathogenic bacteria and viruses, both in the upper respiratory tract and down in the gut and in the vagina. IgA deficiency is sometimes due to the person's immune system not producing functional IgA, but it may also be due to the body erroneously producing some other antibodies that remove all IgA, so-called IgA autoantibodies.
Despite the absence of IgA in persons with selective IgA deficiency, there are very few symptoms connected with this immunodeficiency. Up to 1/3 of persons with selective IgA deficiency do not seek medical attention more frequently than persons without IgA defect, and their disease do not hamper their everyday life. However, persons with selective IgA deficiency are at higher risk of having severer courses of illness than people who do not suffer from the defect. They also have a higher incidence of allergies, autoimmune diseases, intestinal infections, and coeliac disease than the normal population.
IgA protects the barriers of the body, and the researchers therefore advanced the hypothesis that IgA deficiency may be connected with a type of disturbance in relation to the bacteria that IgA helps control in the intestine. As the composition of intestinal bacteria is of importance to health, they compared the intestinal bacterial composition in persons with selective IgA deficiency with healthy persons to acquire greater insight into the disease.
Instead of simply comparing a group of persons with selective IgA deficiency with a control group without IgA defect, which is the standard procedure in this type of study, the researchers paired persons with IgA defect with a person from their household. Professor Susanne Brix Pedersen, who participated in the study, elaborates:
"The reason why we've chosen this approach is that when we look at intestinal bacteria, lifestyle, and especially diet, are among the most important factors in defining what kind of bacterial composition we have in our intestine, and these elements are more similar among members of the same household. In this way, we can better check lifestyle effects, which means that we can assess more accurately the causal connection with the IgA defect."
The team behind the study combined the trial design with sophisticated analysis methods of the function of the microbiota and found that persons with selective IgA deficiency generally have a higher incidence of E. coli, and that there are several intestinal factors which have a correlation with inflammatory and pathogenic processes. But the researchers also went a little deeper and looked at whether they could see a difference in the intestinal microbiota depending on whether there was an actual IgA deficiency, or whether the patient himself/herself produced IgA antibodies. Susanne Brix Pedersen elaborates:
"When people produce antibodies to IgA, this is an autoimmune reaction in which the body's immune system attacks parts of itself. We found that the people who produce these autoantibodies have a composition of intestinal bacteria that increases the risk of infection. At the same time, the immune system is constantly in alert mode, because new IgA antibodies are continuously being produced, which it believes it must fight and this wears down the body."
The study therefore shows that when doctors screen patients with recurrent infections for whether they have an IgA defect, it will be expedient also to clarify which type of IgA defect they suffer from. In this way, they can identify the patients who should be monitored particularly closely because they are at greater risk of having a more severe course of illness.
That the correlation can be serious is shown in the study Association between selective IgA deficiency and COVID-19 published in Clinical Biochemistry and Nutrition, where Japanese researchers ascertained a clear correlation between deaths caused by COVID-19 and IgA deficiency.
More information: Janne Marie Moll et al, Gut Microbiota Perturbation in IgA Deficiency Is Influenced by IgA-Autoantibody Status, Gastroenterology (2021). DOI: 10.1053/j.gastro.2021.02.053
Journal information: Gastroenterology
Provided by Technical University of Denmark