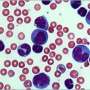
The chemotherapy treatments necessary to treat Acute Myeloid Leukemia (AML) in children can be grueling on the body, and can cause health-related complications during therapy, as well as long down the road after remission. Children receiving chemotherapy for AML receive 4 to 5 intensive chemotherapy courses, and while some children recover quickly from each course, others may take several months or more, which increases their risk for life-threatening infections.
In a recent paper published in The Journal of Clinical Oncology, researchers from Baylor College of Medicine, Children's Oncology Group, University of Southern California, Hospital for Sick Children, Children's Mercy Hospitals and Clinics and University of Washington School of Medicine, discovered a way to predict which children are at highest risk for delayed recovery, a finding that may have significant implications for treatment-related morbidity and mortality.
The paper examines the role of telomeres in blood count recovery, particularly how the length of a patient's telomeres can indicate the rate of white blood cell recovery following chemotherapy treatment.
"Telomeres are the protective caps on chromosome ends that keep DNA from fraying as you age, much like the plastic end of a shoelace prevents it from unraveling. We were interested in telomere length as a marker of blood count recovery, because defects in telomere maintenance are known risks for bone marrow failure and aplastic anemia," said Dr. Maria Monica Gramatges, assistant professor of pediatric oncology at Baylor College of Medicine. "We know that up to 15-20% of children can take two months or longer to recover their blood counts after a course of AML chemotherapy. Our goal was to understand if these children had an underlying genetic predisposition associated with an impaired capacity for recovery."
Gramatges and her colleagues hypothesized that short remission telomere length could be associated with a delay in blood count recovery in children receiving therapy for AML.
Gramatges obtained remission bone marrow samples following the first chemotherapy course from AML patients who recovered as expected (within 30 days) after each chemotherapy course, and from AML patients who experienced significant delays after chemotherapy. She then measured telomere length on each subject and categorized the group by quartile, from shortest to longest.
Subjects in the shortest telomere length quartile took the longest to recover, especially during the last two courses of chemotherapy, with some in that group not even recovering at all.
These findings support the hypothesis that telomeres are an indicator of capacity for blood count recovery following chemotherapy treatment.
Gramatges hopes the results of the AML project will be helpful in further understanding which children are at a higher risk for prolonged myelosuppression (low blood counts), and how to target those children at the highest risk for slow recovery with modified treatments, improved supportive care, and closer monitoring in order to prevent potential complications such as severe infections.
"A significant proportion of children with AML suffer from treatment-related toxicities, with some succumbing to complications of the therapies we give, rather than from the actual cancer itself," says Gramatges. "We hope this research will help us identify those who are at a higher risk for delayed recovery and use this knowledge to reduce the morbidity and mortality associated with AML treatment."
More information: R. B. Gerbing et al. Shorter Remission Telomere Length Predicts Delayed Neutrophil Recovery After Acute Myeloid Leukemia Therapy: A Report From the Childrens Oncology Group, Journal of Clinical Oncology (2016). DOI: 10.1200/JCO.2016.66.9622
Journal information: Journal of Clinical Oncology
Provided by Baylor College of Medicine