Among patients with stage IV melanoma who were being treated with the immunotherapeutic pembrolizumab (Keytruda), the ratio of a particular subset of immune cells in the blood to tumor burden correlated with clinical response, according to data presented at the Second CRI-CIMT-EATI-AACR International Cancer Immunotherapy Conference: Translating Science into Survival, held Sept. 25–28.
Pembrolizumab was approved by the U.S. Food and Drug Administration for treating metastatic melanoma in September 2014. Although some patients have remarkable and durable responses to treatment, the majority do not, according to Alexander Huang, MD, a clinical fellow in the Division of Hematology/Oncology and Institute for Immunology at the Perelman School of Medicine at the University of Pennsylvania in Philadelphia.
"We set out to investigate whether we could monitor and predict a patient's response to pembrolizumab by tracking the effect of pembrolizumab on immune cells in blood samples from the patients," said Huang. "We found that we could, which is important because it opens up the possibility that we might one day be able to use blood-based assays to inform clinical care. However, we need to validate our findings in a larger group of patients before this can become a reality."
Huang and colleagues analyzed blood samples from 29 patients with stage IV melanoma taken before and at 3, 6, 9, and 12 weeks after starting treatment with pembrolizumab. They measured levels of the proliferation marker Ki67 in immune cells called exhausted-phenotype CD8-positive (CD8+) T cells.
"After a prolonged battle with tumor cells, CD8+ T cells become progressively more dysfunctional, or exhausted," said Huang. "Exhausted-phenotype CD8+ T cells have high levels of the protein PD-1 on their surface. Pembrolizumab targets PD-1. In preclinical models, pembrolizumab targeting of PD-1 can reinvigorate exhausted-phenotype CD8+ T cells, something that we can measure by increased levels of proliferation markers like Ki67."
The researchers found that levels of Ki67 were significantly greater in CD8+PD-1+ T cells (exhausted-phenotype CD8+ T cells) in posttreatment blood samples compared with pretreatment blood samples for 78 percent of patients. A clinical response, as measured by immune-related RECIST criteria, occurred in 38 percent of patients.
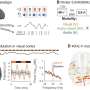
Huang and colleagues measured the level of Ki67 in CD8+PD-1+ T cells before and after treatment, with the peak Ki67 after treatment considered the measure of the extent of reinvigoration of exhausted-phenotype CD8+ T cells. They then found that the ratio of CD8+PD-1+ T cell reinvigoration to pretreatment tumor burden correlated with clinical response. In one cohort of patients, all those who had a ratio greater than 1.94 were alive after 11 months of follow-up compared with 50 percent of patients with a ratio of less than 1.94. In a second cohort, 75 percent of patients with a ratio greater than 1.94 were alive at two years, compared with 29 percent with a ratio less than 1.94.
"We were excited to find that patients with a balance in favor of the immune response compared to tumor burden were more likely to have clinical benefit," said Huang. "If validated in larger studies, this could provide a way to predict early on after starting pembrolizumab treatment whether a patient should continue this treatment or either change to a different treatment or add an additional treatment.
"The fact that we were able to track the immune effect of pembrolizumab in the peripheral blood of patients opens up many doors in terms of research opportunities," added Huang. "We want to put our findings in context with what is known about other biomarkers of response, such as tumor PD-L1 expression."
According to Huang, the main limitation of the study is the small sample size, which means that the correlation between response to pembrolizumab and the ratio of exhausted-phenotype CD8+ T cell reinvigoration to tumor burden needs to be validated in a larger cohort of patients.
Provided by American Association for Cancer Research