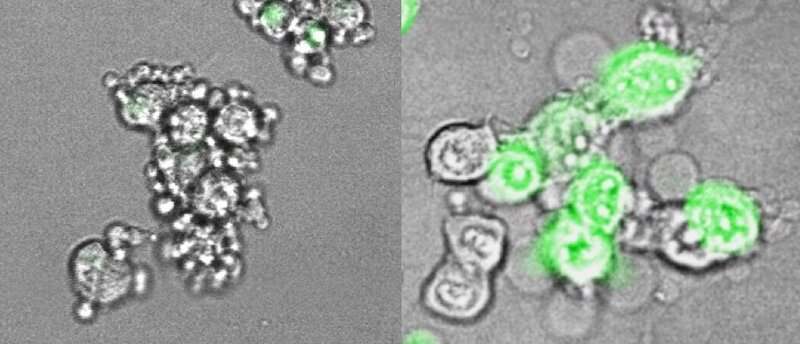
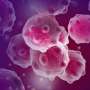
At left, cancer cells from an immunologically 'cold' tumor, in which gasdermin E has been suppressed, undergo a slow, uneventful death. Their outer membrane remains intact and they quietly shrink. The cancer cells at right have had gasdermin E re-introduced: they blow up, forming giant membrane balloons, and release molecules that trigger inflammation and a protective immune response. Credit: Zhibin Zhang/Lieberman Lab, Boston Children's Hospital
Tumors have figured out various ways to prevent the immune system from attacking them. Medicine, for its part, has fought back with cancer immunotherapies. The major approach uses checkpoint inhibitors, drugs that help the immune system recognize cancer cells as foreign. Another method, CAR T-cell therapy, directly engineers peoples' T cells to efficiently recognize cancer cells and kill them.
But not all patients benefit from these approaches, which work for just a minority of cancer types, and CAR T-cell therapy carries significant risks. New research from Boston Children's Hospital, published March 11 in Nature, adds another strategy to the arsenal, one that could potentially work in more types of cancer. It reactivates a gene called gasdermin E, harnessing an immune response we already have but that is suppressed in many types of cancer.
"Gasdermin E is a very potent tumor suppressor gene, but in most tumor tissues, it's either not expressed or it's mutated," says Judy Lieberman, MD, Ph.D., of the Program in Cellular and Molecular Medicine (PCMM), the study's principal investigator. "When you reactivate gasdermin E in a tumor, it can convert an immunologically 'cold' tumor—not recognized by the immune system—into a 'hot' tumor that the immune system can control."
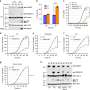
In the study, Lieberman and colleagues showed that 20 of 22 cancer-associated mutations they tested led to reduced gasdermin E function. When they re-introduced gasdermin E in a mouse model, they were able to trigger pyroptosis and suppress growth of variety of tumors (triple-negative breast tumors, colorectal tumors, and melanoma).
Heating up the immune response
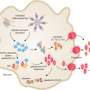
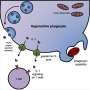
The team also showed, in mouse tumor cell lines, how gasdermin E works. Normally, when cells die, including most cancerous cells, it's through a process called apoptosis, a quiet, orderly death. But if gasdermin E is present and working, cancer cells go down in flames, through a highly inflammatory form of cell death called pyroptosis.
As Lieberman's team showed in live mice, pyroptosis sounds a potent immune alarm that recruits killer T cells to suppress the tumor. The team is now investigating therapeutic strategies for inducing gasdermin E to rally that anti-tumor immune response.
"What we're suggesting is that if we can turn on the danger signal, which is inflammation, we can activate lymphocytes more fully than with other immunotherapy approaches, and have immunity that is potentially much broader," says Lieberman. "Combining activation of inflammation in the tumor with approved checkpoint inhibitor drugs could work better than either strategy on its own."
More information: Gasdermin E suppresses tumour growth by activating anti-tumour immunity, Nature (2020). DOI: 10.1038/s41586-020-2071-9 , nature.com/articles/s41586-020-2071-9
Journal information: Nature
Provided by Children's Hospital Boston