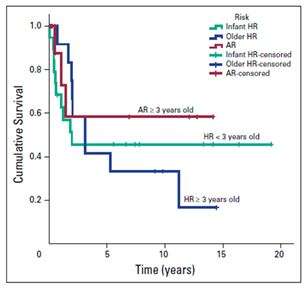
Overall survival of paediatric patients with average-risk (AR) and high-risk (HR) medulloblastoma treated from 1994 to 2013. Credit: American Society of Clinical Oncology
The future of children with brain tumours is very promising. To do nothing is to ignore the very real possibility of a treatment and cure. It is the time now to accelerate clinical and laboratory research in childhood brain tumours.
Brain tumours are the second most common childhood malignancy worldwide. In Malaysia, a nationwide epidemiological survey from 2010 to 2012 found that brain tumours comprise approximately 15% of all childhood neoplasms. The estimated overall incidence of brain tumours amongst Malaysians aged less than 18 years is approximately 9.9 per million per year. After leukemia, brain tumors are the leading cause of cancer deaths in children. Surprisingly, the public remain unaware of the magnitude of this disease. Brain tumours either can be benign or malignant and different proportions of histological subtypes are present in children compared to adults. Medulloblastoma, low grade glioma and ependymoma are the most prevalent paediatric brain tumours. Meanwhile, in children less than 3 years, a third of brain tumours are of the embryonic type. Malignant brain tumours are highly aggressive and may be associated with systemic metastases.
Timely diagnoses with coordinated multidisciplinary team approaches are known to be pivotal factors that lead to increased overall survival and improved quality of life in children with brain tumours. Surgery represents the first line of treatment when addressing paediatric brain tumours. A retrospective review of paediatric patients with medulloblastoma treated in University of Malaya Medical Centre (UMMC) from January 1994 to December 2013 showed 5-year progression-free survival for patients≥ 3 years was 41.7%±14.2% in the high-risk group and 68.6%±18.6% in the average-risk group, whilst the 5-year overall survival in these two groups was 41.7%±14.2% and 58.3%±18.6% respectively. Children younger than 3 years had 5-year progression-free and overall survival rates of 47.6%±12.1% and 45.6%±11.7% respectively. These rates are significantly inferior to those in developed countries. In our series, we postulate a number of contributing factors for this inferior outcome - these include : limited health care resources, inadequate financial support for diagnostic tests and research activities, absence of molecular subgroup information, lack of multidisciplinary neuro-oncology team in many centres, inadequate long-term follow-up and treatment abandonment secondary to cultural beliefs.
At the University of Malaya Medical Centre (UMMC), the care and long-term multidisciplinary follow-up for children with brain tumours are co-ordinated by the Paediatric Hematology-Oncology Unit. The UMMC team follows more than 150 brain tumour patients, from infancy through adulthood in outpatient oncology clinics and approximately 10-15 children and adolescents with brain tumours are diagnosed every year. A multidisciplinary neuro-oncology team was formed in 2013 comprising paediatric oncologists, neurosurgeons, radiotherapists, clinical oncologists, neuropathologists and radiologists. The team discusses both paediatric and adult brain tumour cases at a weekly multidisciplinary conference. They provide the most innovative therapeutic solution in a well-structured multidisciplinary approach, while at the same time offering support to the patient and the family. The departments of neurosurgery, radiation oncology and biomedical imaging have recently expanded their services to include more state-of-the-art equipment and medical facilities, such as gamma knife radiosurgery, conformal radiotherapy and intensity modulated radiotherapy. In addition, paediatric oncologists are able to offer evidence based chemotherapy following protocols from the Children's Oncology Group (COG) and International Society of Paediatric Oncology (SIOP).
While historically the prognosis of brain tumours has been bleak, there is good news on the horizon. The molecular era has advanced our understanding of brain tumour disease biology and identified distinct molecular subgroups with gene expression and DNA methylation, allowing better precision in choice of treatment. This is best exemplified in medulloblastoma which is the commonest childhood malignant brain tumour. The current treatment approach for managing medulloblastoma consists of maximal surgical resection, chemotherapy, craniospinal radiotherapy for older children or a radiotherapy-sparing approach using high-dose chemotherapy for children aged <3 years. Although this 'standard of care' has been effective in improving the outcome of children with medulloblastoma, unfortunately, survivors pay a high price for cure. Impairment in neurocognitive and neuroendocrine functioning, hearing, fertility, cardiopulmonary fitness and physical performance are increasingly recognized late-effects of chemo- and radiation therapy.
To improve treatment precision and reduce unnecessary side-effects, customized and targeted therapies have been implemented for children with brain tumours. These efforts aim to reduce the intensity of treatment for patients with good prognostic molecular signatures in order to decrease morbidity, whilst introducing novel therapies for specific subgroups. For example, in 2016 the World Health Organization (WHO) classification of Tumors of the Central Nervous System has incorporated molecular subgrouping (namely WNT/Wingless (WNT), Sonic Hedgehog (SHH), Group 3 and Group 4) in the diagnosis and management of medulloblastoma. Recent research, identifying mutation in the BRAF gene in brain gliomas, promises new answers as to how and why certain gliomas occur and the ideal treatment strategy for cure. Understanding of the heterogeneity of disease biology amongst the scientific communities worldwide has created a new culture for partnership with medical institutions, government and non-governmental organisations and lay people, without which the chance of finding a cure in brain tumours remains slim.
Paediatric neuro-oncology is an evolving subspecialty in Malaysia. Molecular subgroup typing is not standard practice yet when making a diagnosis. The absence of molecular subgroup information in patients will preclude accurate risk stratification and result in suboptimal treatment. Given the future treatment of childhood brain tumours will require analysis to determine the underlying molecular subgroup in order to correctly risk stratify patients to subgroup specific treatments, understanding the impact of molecular subgroups in brain tumours in Malaysia is a critical first step. To address these gaps and challenges, the paediatric oncology team of University of Malaya has taken several steps.
A brain tumour tissue repository with clinical annotation has been established since 2012 for molecular and genetic studies. Recently, international research collaborations with developed countries have been initiated. The first international brain tumour collaborative project entitled 'Molecular Classification of Paediatric Medulloblastoma in Malaysia' between Telethon Kids Institute, Perth, West Australia and Paediatric Haematology-Oncology Unit in University of Malaya with three other Ministry of Health Hospitals (Penang General Hospital, Sarawak General Hospital and Sabah Woman and Children's Hospital (Likas)) are now underway. The objective of this project is to determine the prognostic significance of the four molecular subgroups of medulloblastoma by DNA methylation profiling (using the 850k methylation array) on diagnostic tumour tissue samples among medulloblastoma children in Malaysia. The aim is to translate the scientific discovery to identify the prognostic factors based on molecular signatures in order to improve the survival and quality of life in future patients.
In addition, a twinning program between University of Malaya and the Princess Margaret Hospital for Children, Perth, Australia will commence in the immediate future with monthly video conference, allowing interactive exchanges with world-renowned brain tumour experts. As brain tumour survivors suffer from significant morbidity following multimodal treatment, a research project focusing on late-effects and quality of life using a self or parent-report "patient questionnaire" is now under planning with International Outreach Program at St. Jude Children's Research Hospital, Memphis, Tennessee, USA to determine the incidence of late-effects in limited resource countries.
With all the genetic and biologic advances in paediatric brain tumours, it is crucial not to lose sight of the importance of prompt diagnosis. Diagnosis of brain tumour is delayed most of the time when compared with other paediatric malignancies. Thus, a retrospective review of delayed diagnosis of childhood brain tumours treated at UMMC from 2000 until 2015 will be undertaken to identify the causes, consequences and potential solutions.
Paediatric neuro-oncology has advanced significantly especially in the past 5 years. Whole genomic analysis of the entire spectrum of paediatric brain tumours has afforded an opportunity to the paediatric neuro-oncology community to reconsider current treatment strategies and design better therapeutic solutions for children with brain tumours. Realistically, however the incorporation of tumour genomic information into "standard" treatment protocols is a major challenge in low and middle income countries due to its high cost. Nevertheless, the paediatric oncology team in University of Malaya will implement several collaborative strategies with international partners over the next 5-10 years to allow children from this region to benefit from personalized therapy for a wide spectrum of brain cancers.
More information: Rajagopal R, et al. Challenges of treating of childhood medulloblastoma in a country with limited resources: 20 years of experience at a single center in Malaysia. Journal of Global Oncology 2017: 3(2):143-156
Provided by University of Malaya