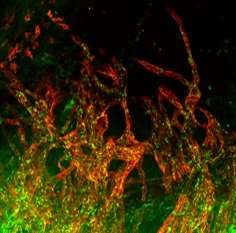
New lymphatic vessel growth, seen under a microscope. Credit: Paul Riley
Researchers funded by the British Heart Foundation have identified how a new treatment in mice can regenerate the heart after a heart attack—preventing the onset of heart failure.
During a heart attack, the heart is starved of oxygen and heart muscle is damaged. The body responds by sending in immune cells to clear up dead and dying cells, but these cells themselves cause further inflammation in the already damaged heart, and this can lead to heart failure. Heart failure is a debilitating condition that affects half a million people in the UK alone.
The team from the University of Oxford found that injecting a protein called VEGF-C after heart attacks in mice significantly reduced the amount of damaged heart muscle, and allowed the heart to recover almost all of its pumping function. In comparison, untreated mice lost almost half of their heart function after a heart attack.
The VEGF-C treatment promoted growth of a network of vessels which are part of the lymphatic system. The research team from the University of Oxford, led by BHF Professor Paul Riley, have now discovered that the extra lymphatic vessels allow the immune cells to be quickly cleared after helping to repair and clear dying and dead cells, but before they can cause significant damage from inflammation. This treatment led to better healing in the heart and better recovery of the heart's pumping function after a heart attack.
When the heart's ability to use the lymphatic system to clear away the immune cells was hampered, more scarring developed, the muscle could not pump as well, and the whole heart started to change shape in response to the damage.
The research team also think that by clearing away macrophages, the first line of immune cells that start the healing process, other immune cells called Tregs could then be allowed into the injured muscle, to further help the heart to repair and recover.
Future research and treatments will focus on achieving the best balance of immune cells after a heart attack to ensure initial heart repair doesn't escalate to inflammation, scarring and heart failure.
The findings were published today in the Journal of Clinical Investigation.
BHF Professor of Regenerative Medicine Paul Riley leads the BHF Centre of Regenerative Medicine in Oxford and Cambridge and led the research. He said:
"We started looking at the lymphatic system in the heart a few years ago—we could never have known how pivotal it might turn out to be for heart repair.
"We now know that it's not enough to just get healing immune cells into the heart. We need to boost the routes that remove these immune cells once they've done their job, so that they don't start causing more harm and ultimately contribute to the long-term damage that leads to heart failure.
"This research has allowed us to start a drug discovery programme to develop drugs to promote the growth of lymphatic vessels and quickly clear immune cells. We hope to get a treatment we could give to people after a heart attack within 5-10 years."
Professor Jeremy Pearson, Associate Medical Director at the British Heart Foundation, which funded the research said:
"Someone goes to hospital with a heart attack every three minutes in the UK. Their hearts will have been starved of oxygen, which is why we urgently need to better understand the damage caused when this happens, and how we can repair it.
"Heart regeneration is the 'holy grail' of heart research. By building on their previous work, the team's new findings bring us one step closer to understanding how to turn this into a reality. Exploiting the lymphatic system opens up new opportunities to find treatments that will limit the damage caused by a heart attack and promote regeneration. It's only by funding important research such as this that we can hope to one day end heart failure."
More information: Immunomodulation via the cardiac lymphatic system to improve heart repair, Vieira et al, Journal of Clinical Investigation, 2018.
Journal information: Journal of Clinical Investigation
Provided by British Heart Foundation