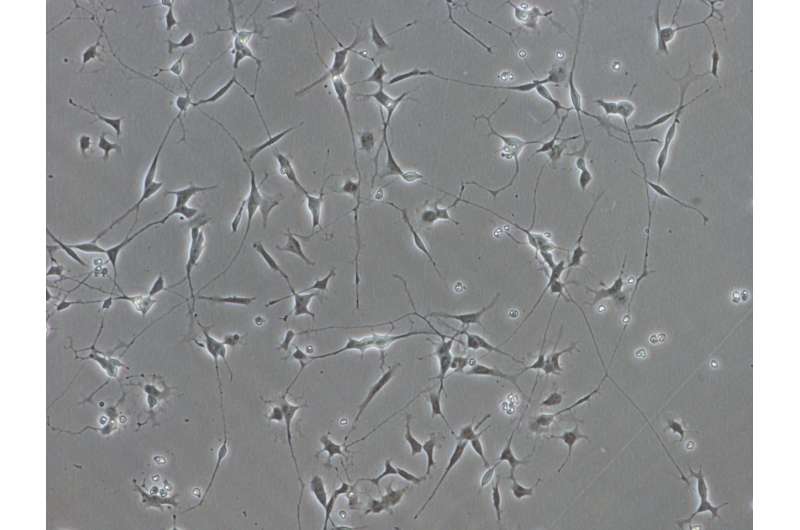
The scientists have found a deficiency in the protein STIM1 in brain tissue from patients with Alzheimer's disease. Its involvement in neurodegenerative processes has been verified thanks to the technique CRISPR/Cas9. Up to now, the effects of a deficiency in this protein critical to sporadic Alzheimer's were not known. Credit: University of Extremadura
The objective of the research, undertaken in the laboratories of the IBPM, is to develop a model for studying Alzheimer's disease (AD) of sporadic origin—in other words, AD that is not due to a hereditary genetic mutation. While Alzheimer's disease of familial or hereditary type is responsible for around 5 percent of all cases, it is thought that 95 percent of incidents are of unknown or sporadic origin.
"In Alzheimer's of family origin, there already exist animal models, because we know which genes are linked to this illness. However, in Alzheimer's disease of unknown origin, to date there are no models that enable us to study how it develops," says Francisco Javier Martin-Romero, one of the authors of the study.
These researchers analysed cultures of damaged brain tissue from a region called medial frontal gyrus, with clinically confirmed alterations provoked by Alzheimer's. These clinical samples were analysed and compared with healthy tissue from patients of the same age. As a result of this comparative study, the scientists found a deficiency in the protein STIM1 in brain tissue from patients with AD.
"We have been working with this protein for 10 years, but we weren't expecting these results with sporadic Alzheimer's," says Martin-Romero. The next step the researchers took was to observe the involvement of this protein STIM1 in the neurodegeneration of the neuron, and they did so using the genetic editing system CRISPR, known popularly as "genetic cut-and-paste." The researchers applied a strategy to eliminate the expression of the gene STIM1 in the neuroblastoma SH-SY5Y cell line, editing the genome with CRISPR/Cas9 using an in vitro model to examine the phenotype of the neuronal cells deficient in STIM1.
"We use the CRISPR technique on a regular basis in the Faculty of Sciences at the UEx, as it has the great advantage that the genome remains stable despite the cuts in the DNA. In this specific case, CRISPR silences the gene that permits the expression of the protein STIM1 in the neuron. Thus, we were able to simulate what occurs in the neuron without this protein, and we observed alterations very similar to those seen in tissues with Alzheimer's," the researcher says. Up to now, the effects of a deficiency in this protein critical to sporadic Alzheimer's were not known, and so this research offers a new biomarker for the illness, an indicator of the progression of the neurodegenerative process.
One of the alterations observed due to the deficiency of STIM1 is in the transport of calcium ions through the plasma membrane of the neurons. "This calcium is necessary for the cell to be fully viable, and an alteration in this process affects its entire physiology, finally causing its death. The cell is unable to halt the transport of calcium, which becomes unregulated and out of control," says Martin-Romero. The investigator says that this transport takes place through calcium ion channels regulated by a voltage. These L-type voltage-gated calcium channels can be blocked using pharmaceuticals based on dihydropyridine. In fact, the researchers were able to halt cell death in vitro using pharmaceuticals based on dihydropyridine because of that blocking action, representing an important new finding in the treatment of Alzheimer's.
The next step for the investigators at the IBPM will be to work with pluripotent stem cells and differentiate them into neurons, first for mice and then for humans, to make development of a model possible. This will allow a description of how the absence of stimulus or reduction in the protein STIM1 determines cell aging in sporadic Alzheimer's disease.
More information: Carlos Pascual-Caro et al, STIM1 deficiency is linked to Alzheimer's disease and triggers cell death in SH-SY5Y cells by upregulation of L-type voltage-operated Ca2+ entry, Journal of Molecular Medicine (2018). DOI: 10.1007/s00109-018-1677-y
Provided by University of Extremadura