Researchers provide definitive proof of where, how blood stem cells are created
Stem cell researchers at UCLA have proven definitively that blood stem cells are made during mid-gestational embryonic development by endothelial cells, the cells that line the inside of blood vessels.
While the anatomic location in the embryo where blood stem cells originate has been well documented, the cell type from which they spring was less understood. The UCLA finding, published in the Dec. 4, 2008 issue of the journal Cell Stem Cell, puts to rest a long-standing controversy over whether blood stem cells were created, or born, in the endothelium or originated from another cell type in a nearby location.
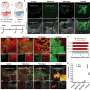
Researchers from the Eli and Edythe Broad Center of Regenerative Medicine and Stem Cell Research at UCLA used a cell fate tracing technique to identify the source of blood stem cells. They genetically marked endothelial cells to discover what other cells they gave rise to and where those cells migrated to in the body.
"We genetically traced the endothelial cells to find out what they became over time," said Luisa Iruela-Arispe, senior author of the paper, a professor of molecular, cell and developmental biology and director of the Cancer Cell Biology Program Area at UCLA's Jonsson Comprehensive Cancer Center. "In that way, we were able to understand that, within the embryo, endothelial cells were responsible for the generation of blood stem cells. They make blood, they aren't just the pipes that carry it."
The finding ultimately could lead to new therapies for certain blood disorders and cancers, said Ann Zovein, the first author of the study and a California Institute for Regenerative Medicine-Broad Stem Cell Research Center Training Grant postdoctoral fellow in Iruela-Arispe's lab.
Blood stem cells currently cannot be grown outside of the body without losing their "stemness," meaning they then differentiate into the different cells that make up blood, including red blood cells, white blood cells and platelets. If blood stem cells can be gown outside the body from endothelial cells and only self-renew, or make more of their own kind, researchers may one day be able to reprogram blood vessel cells to produce blood stem cells to replace the bone marrow in transplants or the mutated blood cells that result in diseases like leukemia.
"We found that endothelial cells are capable of making blood stem cells within embryonic areas that prevent differentiation into other lineages," Zovein said. "In trying to understand how blood stem cells arise from the endothelium, we may learn enough to be able to grow pure, designer blood stem cells outside the human body."
For example, researchers may some day be able to take a blood vessel from a patient and grow blood stem cells specific to that patient, which could be used for bone marrow transplantation. Since the blood stem cells originated from the patient, there would be no need to find a matching donor to provide the marrow. The cells also could be used to replace diseased cells that result in cancer, providing a new way to treat malignancies such as leukemia.
The creation of blood stem cells by endothelial cells occurs at a specific time in embryonic development and researchers want to know what takes place biologically during that period, what specific cell signaling pathways are sending the messages to make blood stem cells. Iruela-Arispe and her team hope to mimic the embryonic environment in the lab to create blood cells that don't differentiate.
"Next we need to understand what signaling mechanisms are at work that allow endothelial cells to make blood stem cells," Iruela-Arispe said. "We need to find out how we can program the endothelial cells to make blood stem cells, what's important in the embryonic blood vessel wall that allows for this phenomenon and whether we can reprogram adult blood vessels to do the same thing."
While this study was done in mouse models, Iruela-Arispe and her team will be working with human endothelial cells to confirm their work and further uncover the cell signaling mechanisms in play.
Source: University of California - Los Angeles