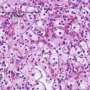
New findings provide more complete picture of kidney cancer
Two recent studies by Van Andel Research Institute scientists are providing a foundation for a more complete understanding of distinct kidney cancer subtypes, which could pave the way for better treatments.
In a study published in Cancer Cell led by Kyle Furge, Ph.D. and Aikseng Ooi, Ph.D., researchers provide a more complete understanding of the biology of Type 2 papillary renal cell carcinoma (PRCC2), an aggressive type of kidney cancer with no effective treatment, which lays the foundation for the development of effective treatment strategies.
Despite obvious morphological, genetic, and clinical differences, hereditary PRCC2 is thought to share similar pathway deregulation due to genetic mutation with its counterpart, clear cell renal cell carcinoma (CCRCC), a subtype that accounts for 75% of all kidney cancers and that, unlike PRCC2, responds favorably to drugs targeting vascular endothelial growth factor (VEGF), a signal protein produced by cells that stimulate blood vessel formation.
The study, which included international collaboration with researchers from the National Cancer Centre Singapore, Génétique Oncologique EPFE-INSERM U753 and Faculté de Médecine Paris-Sud, Le Kremlin-Bicêtre and Institut de Cancérologie Gustave Roussy, Michigan State University, Northwestern Memorial Hospital, Cleveland Clinic, Singapore General Hospital, and The Wistar Institute, identified deregulation of the KEAP1-NRF2 signaling pathway as a factor that distinguishes PRCC2 from CCRCC, but links both hereditary and sporadic PRCC2.
In another study published in Cancer Research, led by Yan Ding, Ph.D., and Bin Tean Teh, Ph.D. and carried out in collaboration with the National Cancer Centre Singapore, researchers integrated gene expression profiling and RNAi screening data to identify genes involved in CCRCC development and progression.
In recent years, several molecularly targeted therapies such as sunitinib, sorafenib, and pazopanib, which target the receptor tyrosine kinases of VEGF have been approved for CCRCC. Although these therapies significantly extend overall survival, nearly all patients with advanced CCRCC eventually succumb to the disease.
Gene set enrichment analysis indicated that cell-cycle-related genes, in particular PLK1, were associated with disease aggressiveness. Further, the association of PLK1 in both disease aggression and in vitro growth prompted researchers to examine the effects of a small-molecule inhibitor in CCRCC cell lines. Their findings highlight PLK1 as a promising potential therapeutic target for CCRCC.