February 29, 2012 feature
Your brain on 'shrooms: fMRI elucidates neural correlates of psilocybin psychedelic state
(Medical Xpress) -- Psychedelic substances have long been used for healing, ceremonial, or mind-altering subjective experiences due to compounds that, when ingested or inhaled, generate hallucinations, perceptual distortions, or altered states of awareness. Of these, the psychedelic substance psilocybin, the prodrug (a precursor of a drug that must in vivo chemical conversion by metabolic processes before becoming an active pharmacological agent) of psilocin (4-hydroxy-dimethyltryptamine) and the key hallucinogen found in so-called magic mushrooms, is widely used not only in healing ceremonies, but, more recently, in psychotherapy as well – but little has been known about its specific activity in the brain.
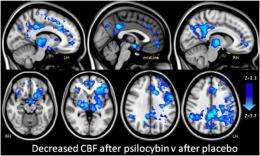
Recently, however, scientists in the Neuropsychopharmacology Unit at Imperial College London used complementary blood-oxygen level dependent (BOLD) functional MRI, or fMRI, in conjunction with a technique for imaging the transition from normal waking consciousness to the psychedelic state. The study found decreased blood flow and BOLD in the thalamus, anterior and posterior cingulate cortex, and medial prefrontal cortex. The researchers concluded that the surprising results strongly suggest that the subjective effects of psychedelic drugs are caused by decreased activity and connectivity in the brain’s key connector hubs, enabling a state of unconstrained cognition.
Lead researcher Dr. Robin L. Carhart-Harris, working in the Neuropsychopharmacology Unit created by Prof. David J. Nutt, recounts the team’s main challenges in establishing an fMRI methodology that would be specific enough to highly correlate neurophysiological activity with the neuronal presence or absence of psilocybin. “There were a number of considerations,” Carhart-Harris tells Medical Xpress. “In terms of experimental design, we had to determine the precise dose and delivery protocol that would be appropriate for obtaining clear fMRI results. “For example,” he explains, “we had to consider temporal dynamics: If the drug was administered orally, the protracted period of time between ingestion, metabolism, and crossing of the blood-brain barrier would fall outside of the short scanning window needed to capture induced brain activity.” They therefore had to rely on intravenous administration.
“Another issue,” Carhart-Harris adds, “was methodological – specifically, isolating any placebo effect derived from changes not due to the injection itself, such as anticipatory anxiety.” The team also had to measure physiological parameters, including breathing and heart rate, in order to use these signals as weighting factors, correlate with baseline levels and remove them as a possible explanation of any observed brain changes.
To address these challenges, Carhart-Harris points to the pilot work the team performed in order to determine the optimal dose. “The original dose was too low in our mock scanner environment, in which subjects were asked to rate regular subjective or perceptual experiences
Regarding next steps in their research, Carhart-Harris sees obtaining a grant to study psilocybin as a treatment for depression – scheduled to begin at the end of 2012 – as key. “Psilocybin decreases brain activity in regions such as the medial prefrontal cortex,” he explains, “that are overactive in depression.” The team may also perform the same investigations with alternative psychedelic compounds, such as MDMA (3,4-methylenedioxymethamphetamine) – a synthetic, psychoactive drug, commonly known as Ecstasy, that is chemically similar to the stimulant methamphetamine.
Carhart-Harris is also interested in the effects of psilocybin on memory. “When subjects are in the scanner,” he illustrates, “and are shown personal memory cues, then asked to close their eyes and remember the emotions at the time of the original event, the recalled emotions are more vivid – indicating elevated brain activation – when under the effects of psilocybin.” Moreover, Carhart-Harris notes that when administered psilocybin when undergoing psychotherapy, there is an increased incidence of sudden personal insights. He speculates that this suggests that psilocybin-induced visual changes indicate that the visual pathways are more sensitive to signals from the hippocampus, which is involved in memory, when under psilocybin.
In addition to depression, Carhart-Harris observes, there are other research and applications that might benefit from the team’s findings. “Those suffering from cluster headaches,” he notes, “report excruciating pain that is difficult to treat, sometimes describing it as worse than the pain childbirth. During such headaches, they show an increase in hypothalamic activity to date has only been ameliorated by deep brain stimulation. However,” he concludes, “when administered psilocybin, they display a decrease in hypothalamic activity and a corresponding suspension of cluster headaches.”
More information: Neural correlates of the psychedelic state as determined by fMRI studies with psilocybin, Published online before print January 23, 2012, doi: 10.1073/pnas.1119598109, PNAS February 7, 2012 vol. 109 no. 6 2138-2143.
Related information:
Implications for psychedelic-assisted psychotherapy: a functional magnetic resonance imaging study with psilocybin, Published online ahead of print January 26, 2012, doi: 10.1192/bjp.bp.111.103309.
Copyright 2012 PhysOrg.com.
All rights reserved. This material may not be published, broadcast, rewritten or redistributed in whole or part without the express written permission of PhysOrg.com.
















