Use of stem cells, conditioning induces immune tolerance
(HealthDay) -- A novel approach using a bioengineered mobilized cellular product enriched with hematopoietic stem cells (HSCs) and tolerogenic graft facilitating cells (FCs) in combination with nonmyeloablative conditioning is safe and practical for inducing immune tolerance after transplantation, according to a study published in the March 7 issue of Science Translational Medicine.
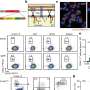
Joseph Leventhal, M.D., from Northwestern Memorial Hospital in Chicago, and colleagues tested an approach to induce immune tolerance in eight individuals, aged 29 to 56 years, receiving human leukocyte antigen-mismatched kidneys and FC/HSC transplants, who underwent conditioning with fludarabine, total body irradiation, and cyclophosphamide. After transplantation, tacrolimus and mycophenolate mofetil were used for immunosuppression.
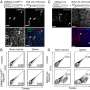
The researchers found that, about one week following transplantation, the absolute neutrophil counts reached a nadir, with recovery by two weeks. At one month, multilineage chimerism ranged from 6 to 100 percent. There was good tolerance of the conditioning, with outpatient management after day two post-surgery. Low-dose tacrolimus monotherapy was given to two patients who exhibited transient chimerism. Two months after transplant, one individual developed viral sepsis and experienced renal artery thrombosis. Durable chimerism, immunocompetence, and donor-specific tolerance were experienced by five subjects, who were successfully weaned off all immunosuppression at one year post-transplant. Anti-donor antibodies were not produced by any of the recipients, nor did any recipient exhibit engraftment syndrome or graft-versus-host-disease.
"These results suggest that manipulation of a mobilized stem cell graft and nonmyeloablative conditioning represents a safe, practical, and reproducible means of inducing durable chimerism and donor-specific tolerance in solid organ transplant recipients," the authors write.
Several of the authors disclosed financial ties to Regenerex and/or are authors on a patent pertaining to the study.
More information:
Abstract
Full Text (subscription or payment may be required)
Editorial (subscription or payment may be required)
Copyright © 2012 HealthDay. All rights reserved.