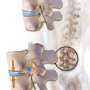
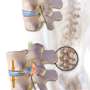
Study questions effect of disc replacement on low back pain
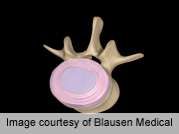
(HealthDay)—Although total disc replacement for chronic low back pain due to degenerative disc disease yields statistically significant improvements compared to conventional fusion, the clinical relevance is unclear and conclusions regarding effectiveness are hampered by low quality evidence and short follow-up, according to a study published in the Jan. 1 issue of Spine.
Wilco C.H. Jacobs, from the Leiden University Medical Center in the Netherlands, and colleagues conducted a systematic literature review and identified seven randomized controlled trials, with a follow-up of 24 months, comparing total disc replacement with any other intervention for chronic low back pain due to lumbar degenerative disc disease.
The researchers found that the included studies had a risk of bias due to sponsoring and lack of blinding. Despite not reaching the predefined threshold, one study that compared disc replacement with rehabilitation identified a significant advantage in favor of surgery. The quality of evidence was low in the six studies that compared disc replacement with fusion and showed a 5.2 mm higher mean improvement in the visual analog scale score of back pain. In five studies also with low quality of evidence, the improvement in the Oswestry disability index score at 24 months was 4.3 points more in the disc replacement group than in the fusion group. The upper bounds of the confidence intervals were below the predefined clinically relevant difference.
"Despite the publication of several recent studies on the effectiveness of total disc replacement, there is a strong need for high-quality studies, with less conflict of interest," the authors write. "Most important are long-term follow-up studies because differences in adjacent segment degeneration will be identified only then."
Copyright © 2012 HealthDay. All rights reserved.