Delivering the best care to the right patient at the right time
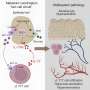
There are two popular models when it comes to delivering the best healthcare – using evidence-based guidelines or applying personalized medicine. Each method has its own merits and drawbacks, but according to one Northwestern Medicine cardiologist, when the two theories are integrated the result is an optimal healthcare delivery model that is both less expensive and better for the patient.
"It should not be one or the other but instead a combination of both," said Jeffrey Goldberger, MD, an attending cardiologist and cardiac electrophysiologist at Northwestern Memorial Hospital and director of Cardiac Electrophysiology Research at Northwestern's Bluhm Cardiovascular Institute.
"My interest in evidence-based medicine and personalized medicine stems from my involvement in the problem the medical community has in identifying patients who are at risk for sudden cardiac deaths. Using the guidelines I outlined in my article, I think we can better treat patients with implantable defibrillators. Based on the research, we are clearly over treating some patients and not treating other patients who would benefit."
Goldberger's research was published in a June 25, 2013 article in The Journal of the American Medical Association (JAMA). Evidence-based medicine dates back to ancient Greece but gained popularity in the 1990s. It consists of basing treatment on the body of clinical data and clinical trials available. Personalized medicine is tailoring medical treatment to the individual characteristics of each patient, focusing on a patient's family history, genetic testing, or other characteristics.
According to Goldberger, who is also a professor at Northwestern University Feinberg School of Medicine, physicians should not follow one theory over the other. Instead, they should bring in personalized medicine to treat those subgroups not helped using evidence-based guidelines, he said.
"For example, many physicians administer a thrombolytic, or clot-dissolving drug, when someone is having a heart attack because the clinical data show those drugs help most patients," Goldberger said. "However, for some older patients these drugs can cause a stroke, so it's best to use personalized medicine to determine the best treatment for these older patients."
"Cultivating a healthcare culture poised to explore these opportunities is critical, but it will entail active participation from a whole range of stakeholders, including physicians, insurers, regulators and healthcare organizations," Goldberger added. "By combining both theories, we have a real opportunity to deliver more precise treatments to the exact patient population who needs it."
In addition to his clinical practice and teaching, Goldberger is an editorial consultant and reviewer for more than 20 medical journals. His clinical interests include pacemakers, cardiac rhythm disorders, catheter ablation, implantable defibrillators and supraventricular tachycardia.
More information: jama.jamanetwork.com/article.a … px?articleid=1691756