New IOM report lays out plan to determine effectiveness of obesity prevention efforts
The United States lags behind other international plans to evaluate obesity prevention efforts, and the country needs to know whether these efforts are having their intended impact, says a new report from the Institute of Medicine. The committee that wrote the report concluded that more systematic and routine evaluations could help determine how well obesity prevention programs and policies are being implemented and which interventions work best. The committee also recommended specific national and community plans for evaluation of obesity prevention efforts.
Investment in obesity program and policy evaluation is too sporadic, presenting serious barriers to understanding the impact of interventions and the need for future investments, the committee said. Moreover, current data monitoring systems inadequately track progress of some programs, and such monitoring is needed at both the national and community levels. Although many monitoring systems exist, the national systems lack adequate leadership, coordination, infrastructure, guidance, accountability, and capacity. Furthermore, local communities do not have the necessary guidance, capacity, data, and resources for assessing the status of obesity, identifying prevention needs, monitoring obesity prevention actions, evaluating their short-term outcomes, and tracking their long-term effects on obesity reduction.
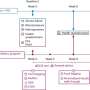
To guide future efforts to inform and improve obesity prevention at the national, state, and community levels, the committee designed separate but interdependent national and community obesity evaluation plans that prioritize activities and leverage existing resources. The plans provide frameworks for obtaining end-user input, choosing indicators and measures for data collection and analysis, and improving the evaluation structure—specifically the success of policy and environmental strategies recommended in the 2012 IOM report Accelerating Progress in Obesity Prevention: Solving the Weight of the Nation.
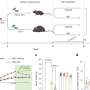
Evaluation efforts lack an agreed-upon set of core indicators that could be used at the national and community levels for measuring and comparing progress in obesity prevention. As a starting point for developing the core set, the committee identified 83 indicators about which data are currently collected that could be incorporated into the national and community evaluation plans and provide guidance to improve the infrastructure and capacities of longer-term evaluations.
The evaluation plans outlined in the report will not be fully realized, however, without coordinated changes across multiple federal, state, and local government agencies and departments in collaboration with other nongovernmental partners responsible for obesity prevention-related activities, the committee said. It recommended the creation of an obesity task force or other entity to oversee and lead the implementation of the national plan and provide support to the community plan. In addition, relevant federal agencies, state and local health departments, and other pertinent organizations should enhance evaluation efforts through improved data collection, common guidance, access to and dissemination of data, work-force ability, capacity to address disparities and health equity, and integration of a systems approach in evaluation efforts.