Breathalyzer technology detects acetone levels to monitor blood glucose in diabetics
A novel hand-held, noninvasive monitoring device that uses multilayer nanotechnology to detect acetone has been shown to correlate with blood-glucose levels in the breath of diabetics. This research is being presented at the 2013 American Association of Pharmaceutical Scientists (AAPS) Annual Meeting and Exposition, the world's largest pharmaceutical sciences meeting, in San Antonio, Nov. 10-14.
Diabetes, which affects an estimated 347 million people worldwide according to the World Health Organization, is an autoimmune disease that prevents the natural cellular uptake of sugar from the blood and often requires continuous blood-glucose monitoring. Current technology, such as the blood glucose meter, is invasive and causes discomfort to patients, often resulting in low compliance. This in turn can ultimately lead to poor health outcomes.
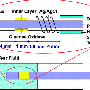
Ronny Priefer, Ph.D., of Western New England University, created the multilayer technology using nanometer-thick films consisting of two polymers that react with acetone. This crosslinks the polymers and alters the physicochemical nature of the film, which provides a quantification of the acetone and thus the blood-glucose levels.
"Breathalyzers are a growing field of study because of their potential to have a significant positive impact on patients' quality of life and compliance with diabetes monitoring. What makes our technology different is that it only accounts for acetone and doesn't react with other components in the breath," said Priefer. "The breathalyzer we currently have is about the size of a book, but we're working with an engineer, Dr. Michael Rust at Western New England University, to make it smaller, more similar to the size of a breathalyzer typically used to detect blood alcohol content levels."
Other common shortfalls with current attempted breathalyzer technology are inconstant results due to the natural humidity of one's breath, high temperature requirements, and lack of selectivity.
Priefer has two Western New England University clinics lined up to perform controlled testing with patients in late 2014–early 2015. This testing would compare readings from the breathalyzer, finger pricking, and actual glucose levels from drawn blood. Priefer is planning for patients to test the breathalyzers in an uncontrolled setting in about two years, keeping a diary of their readings and reporting back.