Where you live can literally shape your body

Whether you live downtown or in the suburbs could have a surprising effect on your bodyweight and your health, with roots running deeper than income differences, says a recent study carried out on data gathered in the canton of Geneva.
Instead of going on a diet, why not leave the suburbs and move downtown to drop some weight? In reality, it might not be quite that simple, but a recent study by researchers from the Geneva University Hospitals (HUG) and EPFL has shown that, for adults, place of residence has an impact on body-mass-index, an indicator used to classify people's weight, that goes beyond income levels. Their findings rely on data gathered over 10 years in the canton of Geneva and were published in the journal Nature Nutrition and Diabetes. They highlight the need for a fine-grained assessment of public health and provide insights that could help guide campaigns to prevent obesity.
Public health specialists long ago connected the dots between people's socioeconomic context and social networks on their health and obesity rates. In particular, body-mass-index (BMI) – a measure that describes body shape based on height and weight – has been believed to reflect the income and the average BMI of their social circles. As a result, obesity prevention campaigns have typically targeted large swaths of the population in low-income neighborhoods. But the data gathered from thousands of adults and children living in Geneva beg for a subtler interpretation.
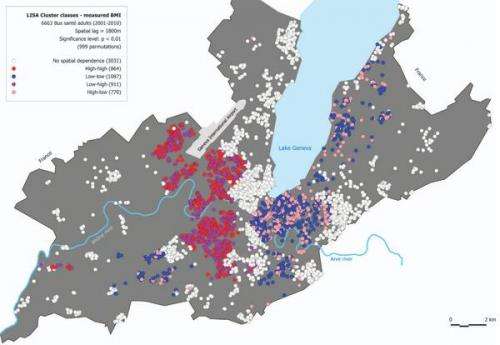
Health data for more than 6600 adults, including measured height and weight, were collected from 2001 to 2010 as part of the Bus Santé population-based study, initiated and carried out by Idris Guessous of the Geneva University Hospitals. The campaign included several units including a mobile examination unit that went to several places in the State to evaluate the health of the canton's residents. The dataset was rounded off with health evaluations of more than 3600 children, obtained in schools across the canton in 2011.
Evaluating these data geographically confirmed that adults' and children's BMI values are not distributed randomly on a map of the canton. Instead, they were found to divide the map into regions with predominantly high or low values, and a larger one where neither trend prevailed. To the south of the Rhone River, the researchers detected a region characterized by low BMI values. North or the Rhone, and to the west of the Praille district, values of high BMI were overrepresented. Between the two, the researchers detected a large "neutral" belt, with a mixed population.
The study revealed two surprising features. First, high adult BMI values did not always overlap with those for children, especially in the heart of the city, north of the Rhone River. And second, at least for adults, the researchers found that differences in income were not enough to explain their findings. But according to the researchers, there are a number other of potential causes, including urban planning, social networks, sport infrastructure, and the promotion of softer forms of mobility, such as walking, biking, or public transportation. In the future, the researchers from EPFL's Laboratory of Geographical Information Systems, who performed the spatial analysis of the results, will seek to tease out the effect of each of these and other factors on BMI.
The study brings to light the importance of finer-grained analysis of community health, both in terms of to geography and age. Lessons learned will primarily benefit other communities seeking to more accurately analyze the health of their residents. But they will also help those involved in setting up anti-obesity campaigns, allowing them to more accurately tailor adult or child specific interventions to the target audience they aim to reach.















