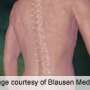
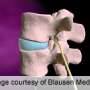
More lumbar Sx complications at teaching hospitals
(HealthDay)—Patients undergoing lumbar spine surgery at teaching hospitals incur longer hospitalizations and have more postoperative complications compared to those treated at nonteaching hospitals, according to a study published in the March 1 issue of Spine.
Sreeharsha V. Nandyala, from Rush University Medical Center in Chicago, and colleagues characterized perioperative complications of 658,616 lumbar spine procedures performed at teaching hospitals (55.9 percent) and nonteaching hospitals. Data were queried from the Nationwide Inpatient Sample (2002 to 2011) for patients undergoing an anterior lumbar interbody fusion, posterior lumbar interbody fusion, anterior/posterior lumbar fusion, or lumbar decompression for the treatment of lumbar degenerative pathology.
The researchers found that patients treated at a teaching hospital were older and had a greater comorbidity burden than the nonteaching group (Charlson Comorbidity Index, 2.90 versus 2.55; P < 0.001). There were significantly more multilevel fusion cases (P < 0.001) at teaching hospitals, and the patients treated there incurred a greater mean length of stay (3.7 versus 3.0 days; P < 0.001). There was also a significantly greater incidence of postoperative pulmonary embolism, deep vein thrombosis, infection, and neurological complications among patients treated at teaching hospitals versus the nonteaching cohort (P < 0.001). Mean total hospital costs and mortality did not significantly differ between the cohorts.
"Despite these differences, the teaching status was not a significant predictor of in-hospital mortality after a lumbar spine surgery," the authors write.
More information:
Abstract
Full Text (subscription or payment may be required)
Copyright © 2014 HealthDay. All rights reserved.