Benefit of aggressive prostate CA Tx weakens as comorbidity rises
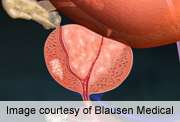
(HealthDay)—For men with early-stage prostate cancer, the cancer-specific survival benefit associated with aggressive prostate cancer treatment is reduced with increasing comorbidity, according to a study published online May 13 in Cancer.
Timothy J. Daskivich, M.D., from the University of California in Los Angeles, and colleagues compared the effectiveness of aggressive versus nonaggressive treatment for reducing cancer-specific mortality in a cohort of 140,553 men aged ≥66 years with early-stage prostate cancer. Data for participants, diagnosed between 1991 and 2007, were extracted from the Surveillance, Epidemiology, and End Results-Medicare database.
The researchers found that, among men with Charlson scores of 0, 1, and 2, but not among those with scores of ≥3, aggressive treatment correlated with a reduced risk of cancer-specific mortality (subhazard ratio for Charlson score ≥3, 0.85; 95 percent confidence interval, 0.62 to 1.18) in propensity-adjusted competing-risks regression analysis. For men with Charlson scores of 0, 1, 2, and ≥3, the absolute reduction in 15-year cancer-specific mortality between men who received aggressive versus nonaggressive treatment was 6.1, 4.3, 3.9, and 0.9 percent, respectively. Aggressive treatment correlated with a lower risk of cancer-specific mortality among men who had well-differentiated and moderately-differentiated tumors with Charlson scores of 0, 1, and 2, but not ≥3 (subhazard ratio for Charlson score ≥3, 1.14; 95 percent confidence interval, 0.70 to 1.89). When considering only well- and moderately-differentiated tumors, the absolute reduction in 15-year cancer-specific mortality was 3.8, 3.0, 1.9, and −0.5 percent for men with Charlson scores of 0, 1, 2, and ≥3, respectively.
"The cancer-specific survival benefit from aggressive treatment for early-stage prostate cancer diminishes with increasing comorbidity at diagnosis," the authors write.
One author is a cofounder of Wiser Care.
More information:
Abstract
Full Text (subscription or payment may be required)
Copyright © 2014 HealthDay. All rights reserved.