Preterm birth breakthrough as antibiotic penetrates placenta
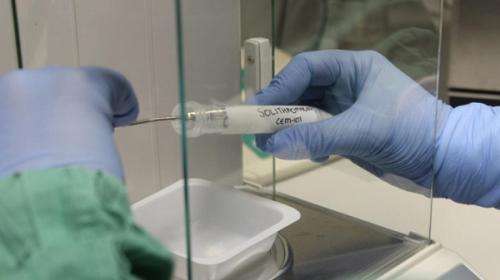
Premature babies would be the main beneficiaries of a new generation antibiotic—solithromycin—that has potential to cross the placenta and kill infections responsible for many preterm births.
It is estimated one in 12 Australian babies is born preterm and almost 15 million born worldwide annually. In Australia the cost for their care is estimated at $500 million a year.
The role of intrauterine infection and inflammation is well recognised; researchers hypothesise vaginal microorganisms break the cervical barrier, colonise the fetal membranes and eventually infect the amniotic cavity. The vigorous inflammatory response that follows ultimately results in preterm birth.
UWA Professor Jeffrey Keelan, based at King Edward Memorial Hospital, has described as 'unprecedented', solithromycin's ability in trials to reach the amniotic cavity and potentially eradicate all preterm birth-associated bacteria from the reproductive tract and foetus.
"In theory we think we can prevent up to 30 per cent of preterm births using solithromycin with the most benefits for the very early pretermers," Prof Keelan says.
"We've done some measurements in sheep and human placentas and estimate the crossover is about 50 per cent compared to just two to four per cent for the older macrolides [antibiotics] and it's 10 to 100 times stronger.
"Our next step is to confirm in pregnant women that the antibiotic crosses the placenta and eradicates harmful bacteria in the reproductive tract."
Full scale clinical trials will run parallel between WA and the USA if a grant application is successful.
Prof Keelan says current antibiotics are largely ineffective in reducing the number of preterm births because they either fail to kill the particular bacteria or don't cross the placenta at effective levels.
Solithromycin has been developed by American company Cempra Inc. specifically to combat antibiotic resistant organisms, initially for the treatment of sexually transmitted diseases and pneumonia but with enormous potential in reducing preterm births.
Prof Keelan says Cempra scientists added three molecular groups to its predecessor clindamycin to create solithromycin, meaning organisms sensitive to solithromycin would have to develop three separate mutations in order to become resistant.
The addition of the molecules also changes the way it moves around the body; tests show that 70 per cent of solithromycin taken orally reaches the blood stream, far more than older macrolides.
More information: "Maternal Administration of Solithromycin, a New, Potent, Broad-Spectrum Fluoroketolide Antibiotic, Achieves Fetal and Intraamniotic Antimicrobial Protection In a Pregnant Sheep Model." Jeffrey A. Keelan, Matthew W. Kemp, Matthew S. Payne, David Johnson, Sarah J. Stock, Masatoshi Saito, Prabhavathi Fernandes, and John P. Newnham. Antimicrob. Agents Chemother. AAC.01743-13; published ahead of print 4 November 2013, DOI: 10.1128/AAC.01743-13