Common gut microbes may contribute to obesity
A link between obesity and the microbial communities living in our guts is suggested by new research at Washington University School of Medicine in St. Louis. The findings indicate that our gut microbes are biomarkers, mediators and potential therapeutic targets in the war against the worldwide obesity epidemic.
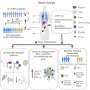
In two studies published this week in the journal Nature, the scientists report that the relative abundance of two of the most common groups of gut bacteria is altered in both obese humans and mice. By sequencing the genes present in gut microbial communities of obese and lean mice, and by observing the effects of transplanting these communities into germ-free mice, the researchers showed that the obese microbial community has an increased capacity to harvest calories from the diet.
"The amount of calories you consume by eating, and the amount of calories you expend by exercising are key determinants of your tendency to be obese or lean," says lead investigator Jeffrey Gordon, M.D., director of the Center for Genome Sciences and the Dr. Robert J. Glaser Distinguished University Professor. "Our studies imply that differences in our gut microbial ecology may determine how many calories we are able to extract and absorb from our diet and deposit in our fat cells."
That is, not every bowl of cereal may yield the same number calories for each person. People could extract slightly more or slightly less energy from a serving depending upon their collection of gut microbes. "The differences don't have to be great, but over the course of a year the effects can add up," Gordon says.
Trillions of friendly microbes reside in the intestine, where they help to digest food that the body can't on its own, such as the complex sugars found in grains, fruits and vegetables. As part of the digestive process, the microbes break down nutrients to extract calories that can be stored as fat.
The researchers focused on two major groups of bacteria - the Bacteroidetes and the Firmicutes - that together make up more than 90 percent of microbes found in the intestines of mice and humans. In an earlier study, they compared genetically obese mice and their lean littermates. The obese mice had 50 percent fewer Bacteroidetes and proportionately more Firmicutes. Moreover, the differences were not due to a bloom of one species in the Firmicutes or a diminution of a single or a few species of Bacteroidetes: virtually all members of each group were altered.
In one of this week's Nature articles, Ruth Ley, Ph.D., a microbial ecologist in Gordon's group, reports on her investigation into whether these findings also held true among obese humans. She followed 12 obese patients at a Washington University weight loss clinic over a one-year period. Half the patients were on a low-calorie, low-fat diet and half were on a low-calorie, low carbohydrate diet.
At the outset of the study, the obese patients had the same type of depletion of Bacteroidetes and relative enhancement of Firmicutes as the obese mice. As the patients lost weight, the abundance of the Bacteroidetes increased and the abundance of Firmicutes decreased, irrespective of the diet they were on. Moreover, not one particular species of Bacteroidetes but the entire group increased as patients lost weight.
In a companion paper in the same journal, Peter Turnbaugh, a Ph.D. student in Gordon's lab, compared the genes present in the gut microbial communities of the obese and lean mice using the newest generation of massively parallel DNA sequencers.
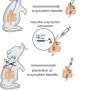
The results of these so-called comparative metagenomic studies revealed that the obese animals' microbial community genome (microbiome) had a greater capacity to digest polysaccharides, or complex carbohydrates. By transferring the gut microbial communities of obese and lean mice to mice that had been raised in a sterile environment (germ-free animals), he confirmed that the obese microbial community prompted a significantly greater gain in fat in the recipients.
Gordon notes that these findings represent steps in a long journey designed to understand the contributions of our microbial self to our health. "Our microbial cells outnumber our human cells by as much as 10 fold and, and they may contain 100 times more genes than our own human genome," Gordon says.
These studies raise a number of questions, according to Gordon. "Are some adults predisposed to obesity because they 'start out' with fewer Bacteroidetes and more Firmicutes in their guts?" he asks. "Can features of a reduced Bacteroidetes-Firmicutes enriched microbial community become part of our definition of an obese state or a diagnostic marker for an increased risk for obesity? And can we intentionally manipulate our gut microbial communities in safe and beneficial ways to regulate energy balance?"
Source: Washington University School of Medicine