Treating obstructive sleep apnea, preventing heart attacks and strokes
Researchers in Brazil have found that treating patients who suffer from obstructive sleep apnea (OSA) with continuous positive airway pressure (CPAP) dramatically reduces early indications of atherosclerosis in just months, linking OSA directly to the hardening or narrowing of the arteries. Until now, no study has demonstrated such a direct relationship between the two.
“OSA is independently associated with increased risk of fatal cardiovascular events that can be reversed by treatment with CPAP,” wrote Luciano Drager, M.D., of the University of São Paulo Medical School in Brazil.
The research was published in the first issue of the American Journal of Respiratory and Critical Care Medicine for October of 2007, published by the American Thoracic Society.
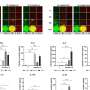
The researchers selected 24 men with severe OSA and no other comorbidities and randomly assigned them to receive either CPAP therapy or no treatment. After establishing the baseline data for each subject, they then tracked several indicators of pre-clinical atherosclerosis, including carotid intima-media thickness (a measure of arterial plaque), pulse-wave velocity (a measure of arterial stiffness), carotid diameter, C-reactive protein (a marker of inflammation), and catecholamine level (a marker of physical stress) over the course of four months.
“[All markers] were similar across the study period in the control group,” wrote Dr. Drager. “In contrast, the group treated with CPAP had a significant decrease in carotid intima-media thickness, pulse-wave velocity, C-reactive protein, and catecholamines.”
While there is a known association between OSA and risk of myocardial infarctions and strokes, the causal connection between OSA and atherosclerosis as the principle mechanism behind those cardiovascular events has proven difficult to establish.
“The majority of patients with OSA share several risk factors for atherosclerosis, including obesity, hypertension, hypercholesterolemia, insulin resistance, and hyperglycemia,” explained T. Douglas Bradley, M.D., and Dai Yumino, M.D., both of the Sleep Research Laboratory at the Toronto Rehabilitation Institute at the Centre for Sleep Medicine and Circadian Biology at the University of Toronto, in an editorial in the same issue of the journal.
Furthermore, while non-randomized observational trials have suggested that the risk of adverse cardiovascular events is lower among patients who accept treatment by CPAP than in patients who do not accept CPAP therapy, it is possible that this difference may be due to better overall adherence to all prescribed treatments in patients who accept CPAP than in those who do not, as opposed to any direct benefit of CPAP itself.
“Whereas physiological studies suggest that OSA provides a substrate for the development of atherosclerosis, and epidemiological and observational studies suggest an association between OSA and odds of having atherosclerosis, there remains a gap between cause and effect yet to be filled,” wrote Drs. Yumino and Bradley. “Drager and colleagues provide evidence that begins to fill that gap.”
Indeed, after four months of CPAP therapy, carotid intima-media thickness declined by nine percent, which is remarkable in light of the fact that in a large-scale study, patients undergoing cholesterol-lowering pravastatin therapy saw carotid intima-media thickness decline by twelve percent after a full year. Other indicators showed similar magnitudes of improvement.
The researchers put forth a number of potential pathways whereby OSA could contribute to atherosclerosis progression, including inflammation, oxidative stress, lymphocyte activation, and high-density lipoprotein dysfunction. “CPAP treatment could reverse several of these pathways,” they wrote.
Still, the investigators caution that, while they are confident in the biological validity of their results, the rigid inclusion criteria makes it difficult to extrapolate their results to different populations, including women, patients with other co-morbidities and patients with mild to moderate OSA.
Source: American Thoracic Society