Stem cells may enhance capability of heart cells to regenerate
During a fatal heart attack, at least 1 billion heart cells are killed in the left ventricle, one of the heart’s two big lower pumping chambers that move blood into the body.
In less severe coronaries, dead cardiac cells are replaced by connective tissue cells that form scar tissue in the damaged heart. But the result is never very satisfactory. Scarred ventricular walls are thin, and don’t contract very well — a problem in a workhorse organ designed for sustained pumping.
Inadequate heart repair concerns British-trained developmental biologist Christine Mummery, who has made cardiac cells her specialty. She’s the Harvard Stem Cell Institute Radcliffe Fellow, and will be in residence at Harvard for a semester. (Most Radcliffe Fellows — who number about 50 a year — stay through May.)
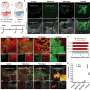
Mummery is group leader at the Hubrecht Laboratory of the Netherlands Institute for Developmental Biology, and a specialist in converting stems cells to heart and vascular cells that act like new ones. Heart cells, Mummery believes, have an untapped regenerative capacity that can be enhanced by transplanting stem cells that grow into efficient heart muscle.
Mummery is interested in using laboratory heart cells as a model for cardiac activity — which someday might help scientists identify novel genes, or screen new drugs inexpensively.
To explain her ideas last week (Sept. 26), Mummery led about 100 listeners through the ABCs of stem cell research. The lecture, in a crowded second-floor colloquium room at 34 Concord Ave., near Radcliffe Yard, was the second in a series of public talks by 2007-08 Radcliffe Fellows.
“I’m going to tell you about stem cells, warts and all,” said Mummery. She also hoped that some scientific grounding in the issue would give her lay audience critical perspective on promising therapies — including medical “breakthroughs” that are nothing of the kind.
A lot of conditions are already popularly associated with stem cell therapy, including Parkinson’s disease and diabetes, said Mummery. But many of them don’t belong in that arena, she said, because too many cells or kinds of cells are affected. Among the conditions unlikely to be mitigated by stem cell therapies are Alzheimer’s, stroke, and multiple sclerosis (MS).
Stem cells are different from other cells in the human body because they can change — “differentiate” — into other cell types. This variability makes stem cells exciting, since they could in theory replace damaged or defective cells.
There are two basic types, explained Mummery, whose Radcliffe talk was illustrated with slides of pictures, graphs, and text.
Adult stem cells, from bone marrow and elsewhere, do not present ethical problems. They can be used — though with difficulty — in conditions affecting the skin, hair, pancreas, bone, and perhaps the brain and heart. But there are too few adult stem cells to do much good, she said. They also change unreliably, and only into a limited number of other cell types.
On the other hand, embryonic stem cells “are ethically very sensitive,” said Mummery, because the embryo has to be destroyed to harvest them. But these versatile cells can transform into all of the human body’s 200 cell types.
Adult stem cells are close to being used in human clinical applications for brittle (unstable) diabetes, for making bone and cartilage, and for skin cell transplantation. But for heart disease, so far, adult stem cells have been a bust.
Skeletal muscle stem cells transplanted into the heart sometimes cause cardiac rhythms to go haywire. And injecting bone marrow cells into the heart carries the risk of creating bone matter there. After four clinical trials on humans, said Mummery, “we haven’t solved the problem of where we’re going to get contractile heart cells from.”
Cord blood — blood that remains in the umbilical cord and placenta after birth — is talked about in the press as a source of embryonic-like blood cells, said Mummery. For a price, some European firms will even store cord blood in hopes of medical advances.
But there is never enough to “treat more than a child,” said a skeptical Mummery. Cord blood — likely storable for up to 15 years — is also impractical for adult conditions, like heart disease, which occur much later in life. Still, bogus stem cell “treatments” are still out there, said Mummery — for MS (in Turkey, using untested cord blood) and amyotrophic lateral sclerosis (in China, using fetal olfactory neurons).
In the Netherlands, Mummery has induced heart attacks in mice, then injected human cardiac cells into the affected area. Grafts developed, and new cells survived for more than six months — “but we still cannot cure a mouse,” said Mummery. “Why? That’s one of the reasons I’m here [at Harvard],” she said.
Twice a week she works with researchers at Massachusetts General Hospital. This month, they’ll start a series of experiments transplanting cells into mouse hearts. They’ll use human adult cardiac progenitor cells, which are undifferentiated and have some capacity for self-renewal. And endothelial cells from the lining of blood vessels, which form pavement-like layers of tissue and are thought to be strongly adaptive.
Mummery will also use her time as a Radcliffe Fellow to work with Kevin Kit Parker, an assistant professor of biomedical engineering at the Harvard School of Engineering and Applied Sciences, where he directs the Disease Biophysics Group.
Their working hypothesis: Cells transplanted to the heart do not exact enough force, and may be too isolated to be effective. Mummery and Parker will investigate how the shape of a transplanted heart cell affects its electrical properties — and therefore the relative force of heart contraction.
“The idea is to exchange materials and ideas,” said Mummery of her dual experiments while at Harvard. She’ll visit again in the spring.
Source: Harvard University