Immune deficiency and balance disorder result from single gene defect
A genetic defect that causes a severe immune deficiency in humans may also produce balance disorders, according to a new study by researchers at the University of Iowa, The Jackson Laboratory and East Carolina University.
The study, published online Feb. 21 in the Journal of Clinical Investigation, examined a specialized strain of Jackson Laboratory mice with a mutation that eliminates the production a protein called p22phox. Disruption of this protein causes a form of chronic granulomatous disease (CGD) -- a severe immune deficiency -- in humans.
The researchers found that mice without p22phox develop an immune deficiency that mimics human CGD. They also discovered that the gene defect produces a severe balance disorder in the mice caused by loss of gravity-sensing crystals in the inner ear.
"The implication is that human patients with CGD caused by defects in this gene may also have balance disorders," said Botond Banfi, M.D., Ph.D., UI assistant professor of anatomy and cell biology and senior author of the study. "If that is the case, this would be the first patient population where we could study the consequences of losing the sensation of gravity.
"We hope that clinicians will test the balance capacity of those patients with this rare form of CGD" Banfi added. "Although it is hard to say what the consequences might be of not sensing gravity, these patients may be more prone to accidents like falling."
In addition to Banfi, the research team included Yoko Nakano, Ph.D., a UI postdoctoral fellow in Banfi's laboratory and lead author of the study; David Bergstrom, Ph.D., research scientist, and Chantal Longo-Guess, research assistant, both at The Jackson Laboratory; Sherri Jones, Ph.D., associate professor of communication sciences and disorders at East Carolina University; and William Nauseef, M.D., UI professor of internal medicine.
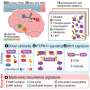
P22phox is emerging as a critical subunit of a family of enzymes that produce reactive oxygen species (ROS). For many years, ROS were simply thought of as destructive molecules that can kill infecting bacteria but also damage human cells. More recently, however, ROS have been shown to play an important role in many normal cell processes, including development and blood pressure regulation. The family of enzymes that produce ROS are called NADPH oxidases (Nox), and disruption of these enzymes has been implicated in a range of diseases, including cardiovascular and neurodegenerative diseases as well as immune deficiencies like CGD.
There are several forms of CGD caused by different genetic defects affecting the Nox complex of pathogen-fighting cells called phagocytes. CGD caused by lack of p22phox is one of the least common forms of the disease in humans. The mutant mouse, which was produced by The Jackson Laboratory's Neuromutagenesis Facility, represents the first animal model for this version of CGD and will be helpful in understanding the disease and developing potential treatments.
The study found that the mice without the p22phox protein were unable to produce ROS in phagocytes and were particularly susceptible to infection. For mice without the protein, infection with bacterial pneumonia was universally fatal. In contrast, normal mice had a 100 percent recovery rate from the same infection.
The mutant mice also had a severe balance disorder. Unlike normal mice that quickly learned how to walk on a rotating rod without falling off, the mutant mice always fell off within a few seconds. Additionally, the study showed that activity of nerve cells in the inner ear responsible for sending gravity signals to the brain was absent in the mutant mice.
"Loss of p22phox affects two enzyme complexes: one in phagocytes that is responsible for the immune defect, and one in the inner ear," Banfi said. "Since this is the first mouse model for defects in the p22phox subunit, this is the first time that its role in balance has been revealed."
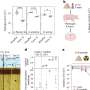
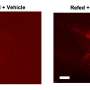
Although inner ear cells looked normal in the mutant mice, the researchers discovered that otoconia -- tiny calcium carbonate crystals that are essential for sensing gravity -- do not form in the inner ears of these mice. Restoring the normal gene to the mutant mice rescued otoconial production and prevented the balance disorder. However, although the treatment did improve the mice's immune response, the partial restoration of gene expression was not sufficient to cure the immune deficiency completely.
"This may mean that gene therapy, which would only partially restore expression of p22phox, would not completely cure CGD in humans," cautioned Banfi. "We may have to look for alternatives and these mice will be ideal models to test new ideas for therapy."
The team was also able to track the location of the Nox complex during embryonic development of the inner ear by visualizing the location of p22phox. Interestingly, the complex does not reside in the same place that the otoconia form leading the researchers to propose a new mechanism by which the Nox complex controls production of the crystals.
"We speculate that superoxide radicals generated by the p22phox–containing complex facilitate the formation of otoconia by producing the right conditions, high pH and high calcium concentration, in the compartment where these calcium carbonate crystals form," Banfi explained.
Source: University of Iowa