A new gene trigger for pregnancy disorder identified
The COMT gene – known already for its role in schizophrenia – has been found to play a role in preeclampsia, according to a report in today’s advance on-line issue of Nature.
Led by researchers at Beth Israel Deaconess Medical Center (BIDMC), the study further suggests that a steroid molecule, 2-ME, may serve as both a diagnostic marker and therapeutic supplement for the treatment of this dangerous pregnancy disorder.
Characterized by hypertension, proteinuria, and edema, preeclampsia affects approximately 5 percent of all pregnancies worldwide, and is a leading cause of maternal and neonatal morbidity. Knowing that placental hypoxia, or oxygen shortage, associated with vascular dysfunction, is a hallmark of the condition, senior author Raghu Kalluri, PhD and his colleagues began by screening for genes that regulate hypoxia.
“Seeing pregnant women with this disease in the clinic inspired me to dedicate our efforts to find likely causative genes that play a role in preeclampsia,” says Kalluri.
“During pregnancy, hypoxia is associated with the formation of new blood vessels,” explains Kalluri, Chief of the Division of Matrix Biology at BIDMC and Professor of Medicine at Harvard Medical School.
“As a result, during the first trimester of pregnancy, when the fetus is undergoing rapid development, hypoxia levels are high. As the pregnancy progresses, hypoxia levels should naturally come down as fetal blood vessels formation slows.” But, he adds, for unknown reasons, patients with preeclampsia remain hypoxic well into their third trimester of pregnancy.
Studies in the Kalluri laboratory revealed an enzyme known as COMT (catechol-O-methyltransferase) in preeclampsia, a gene commonly associated with schizophrenia which, under normal circumstances, inactivates the catecholamine class of neurotransmitters.
“Interestingly, this enzyme contributes to the breakdown of estrogen into 2ME (2-methoxyestradiol), a metabolite that suppresses the activity of hypoxia inducible factor protein,” explains Kalluri. “We wondered if, in cases of preeclampsia, COMT was not functioning properly. In support of this hypothesis, we found that COMT levels were deficient and 2-ME levels were lower in pregnant women with preeclampsia.”
Next the investigators looked at genetically engineered COMT deficient mice; as predicted, the animals failed to produce 2-ME. At 14 weeks gestation – the presumable equivalent of the beginning of the third trimester in human pregnancy – the animals developed protein leak in the urine, high blood pressure and problems with placental blood vessels associated with decreased oxygen levels.
In addition, the animals delivered a day or so earlier than normal pregnant mice and there was a greater incidence of stillborn pups. However, once the pups were delivered, the health of the mother returned to normal.
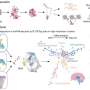
“The loss of 2-ME likely sets in motion a cascade of events culminating in preeclampsia,” says Kalluri. “Disruption of COMT/2-ME led to elevated hypoxia, leading to angiogenic dysfunction and placental insufficiency, which then results in a further decrease in 2-ME levels.”
In the final portion of the study, the authors administered 2-ME to the mice, resulting in a reversal of preeclampsia-like-symptoms.
“Interestingly, the many diverse factors that have been identified in the recent years as elevated or suppressed in women with preeclampsia are fixed by 2-ME, suggesting that this action of COMT is central to proper vascular function in the placenta,” notes Kalluri. “This study offers the possibility of screening for COMT gene defects in pregnant women to predict preeclampsia.”
Source: Beth Israel Deaconess Medical Center