As rates rise, researchers find better way to identify melanoma
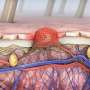
University of Rochester Medical Center researchers found a new protein produced excessively in malignant melanoma, a discovery that is particularly relevant as skin cancer rates climb dramatically among young women.
The protein, IMP-3, is not over-expressed in harmless moles but is increased in the most dangerous types of skin cancer, and in a subset of lesions that can be difficult to predict called thin melanomas. The finding offers a potential target for treatment – but perhaps most importantly might give doctors a new, objective way to distinguish melanoma from some benign moles that look like melanoma but are not cancerous.
"We are very excited about our finding that IMP-3 is an important progression marker in malignant melanoma," said first author Jennifer G. Pryor, M.D., a third-year resident in the URMC Department of Pathology and Laboratory Medicine. "Although we have learned a lot about melanoma in recent years, it has unique biologic properties that sometimes make it difficult to diagnose and to plan for the proper treatment. This protein may have a key role in helping us to understand and distinguish between various types of melanocytic lesions."
The research is published in the journal Modern Pathology. http://www.nature.com/modpathol/journal/v21/n4/full/3801016a.html
This summer the National Cancer Institute warned that new cases of melanoma among young women jumped 50 percent since 1980. Possible explanations, medical experts said, include increased use of tanning beds and more time spent outdoors. Overall rates of melanoma have also been rising among older adults.
The pilot study investigated samples of 56 biopsied lesions from 48 adults. The lesions fell into the category of cutaneous melanocytic neoplasms, a diverse group that includes benign moles; Spitz nevi, a type of mole seen in younger people that can be easily mistaken for melanoma but is not cancerous; and malignant melanoma, which has several phases of growth.
Pathologists play a major role in diagnosing and staging skin cancers, by sorting through neoplasms and identifying features. They analyze cells within the lesions and apply chemical stains and other tools to measure the depth and predict future behavior of the growths.
This study by Pryor and co-authors showed why IMP-3 might be an important tool for pathologists. None of the benign moles or the benign moles with irregular features and some abnormal cells over-expressed the IMP-3 protein. However, the protein was produced excessively in most melanomas, and overly expressed more often in metastatic melanomas.
IMP-3 was also over-expressed in rare cases of invasive thin melanomas. This is significant because most thin melanomas have a good prognosis, but some act more aggressively and currently there is no accurate way to distinguish between the types of thin lesions.
IMP-3 is an insulin-like growth factor-II mRNA binding protein. It is involved in cell proliferation and appears to play a role in tumor formation in a number of cancers.
In previous studies expression of the IMP-3 protein has been linked to pancreas, kidney, ovary and lung cancers, but this is the first published study to demonstrate a connection to melanoma, Pryor said.
Additional research is needed to compare IMP-3 expression with long-term survival data from thin melanoma patients, to find out if patients whose tumors express IMP-3 might benefit from more careful monitoring and aggressive treatment, the study noted.
The antibody used in this research was obtained from the Dako Corporation of California, through a collaborative arrangement initiated by the corresponding author, Haodong Xu, M.D., Ph.D., associate professor of Pathology and Laboratory Medicine at URMC. Xu and his colleagues have previously published studies of IMP-3 as a potential therapeutic target for high grade neuroendocrine carcinomas.
Source: University of Rochester