Protein identified that plays role in blood flow
For years, researchers have known that high blood pressure causes blood vessels to contract and low blood pressure causes blood vessels to relax. Until recently, however, researchers did not have the tools to determine the exact proteins responsible for this phenomenon.
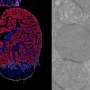
Now, using atomic force microscopy - a microscope with very high resolution - and isolating blood vessels outside the body, University of Missouri researchers have identified a protein that plays an important role in the control of tissue blood flow and vascular resistance. This new knowledge brings researchers one step closer to understanding vascular diseases, such as high blood pressure, diabetes and other vascular problems.
"This study provides new insights that clarify the role of specific proteins and the vascular smooth muscle cells that control the mechanical activity of blood vessels," said Gerald Meininger, professor and director of MU's Dalton Cardiovascular Research Center. "We have identified an important receptor that is responsible for the ability of small arteries in the body. This research provides new clues for the cause of vascular diseases, such as high blood pressure and diabetes and may be used in the future as a possible therapeutic target."
The researchers isolated blood vessels from the body and used atomic force microscopy to apply a controlled force to particular proteins located on the surface of smooth muscle cells from the blood vessel wall. When force was applied to the proteins, the smooth muscle cells reacted, and constricted or contracted depending on the proteins that were targeted. Testing several proteins, researchers were able to pinpoint which proteins played a role in the mechanics of blood vessels.
In 90 to 95 percent of high blood pressure cases the cause is unknown, according to the American Heart Association. Understanding the role of these proteins in controlling blood vessel function will eventually lead researchers to better answers for treating and preventing vascular disease, Meininger said.
Source: University of Missouri-Columbia