Brain disorder suggests common mechanism may underlie many neurodegenerative diseases
A Mayo Clinic-led international consortium has found a mechanism that may help explain Parkinson's and other neurological disorders.
Studying just eight families worldwide, the international team of researchers have discovered a genetic defect that results in profound depression and parkinsonism in a disorder known as Perry syndrome. Although this syndrome is exceedingly rare, the mechanism implicated in it may help explain the origins of a variety of neurodegenerative disorders, such as Parkinson's and amyotrophic lateral sclerosis diseases, and even common depression and sleep disorders that are also hallmarks of the disorder, the researchers say.
In the study, to be published in the February issue of Nature Genetics (online January 11), the researchers report that people with Perry syndrome have mutations in a subunit of the dynactin complex (DCTN1; p150glued), which is essential to the movement of molecular "cargo" inside brain cells, or neurons. In this case, the mutations meant that the cargo was being driven on a "train" that essentially had faulty brakes. And because Perry syndrome resembles many other neurodegenerative diseases, the findings suggest breakdowns along the cell's interior transportation grid may be a common mechanism underlying neurodegeneration.
"Understanding why distinct neurons are selectively vulnerable to neurodegeneration in different brain disorders is one of the greatest puzzles in neuroscience," says the study's lead investigator, Matthew J. Farrer, Ph.D., a professor of neuroscience at Mayo Clinic. "These findings suggest that trafficking of specific cargoes inside brain cells may be a general problem in a variety of neurodegenerative diseases, depression, and other disorders."
"It points us to a unified theory of what is going wrong in many of them," says the study's senior author, Zbigniew K. Wszolek, M.D., professor of neurology at Mayo Clinic.
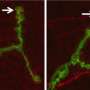
Molecules, vesicles and organelles within a cell are constantly carried via a network of crisscrossing microtubules that act like the tracks of an elaborate railroad system. Because, for the most part, neurons do not regenerate or divide as do other cells in the body, trafficking cargo efficiently over the lifetime of a neuron is fundamentally important, says Dr. Farrer.
Disruptions in this railroad system have been seen in many neurodegenerative diseases, but these problems have been generally regarded as byproducts of the disorder rather than the cause, the researchers say. These new findings may change that view, they say.
For example, in amyotrophic lateral sclerosis (ALS), a motor neuron disease also known as Lou Gehrig's disease, the molecular motors (for example, dynein, dynactin and kinesin) that drive transport from distant nerve terminals to the cell body may become defective. In some forms of Parkinson's disease, growing evidence indicates that the cargoes being trafficked are also misdirected by faulty signaling, due to pathogenic mutations in the leucine-rich repeat kinase 2(LRRK2) gene, Dr. Farrer says.
The findings may also shed light on other neurodegenerative disorders, the researchers say. In Alzheimer's disease, frontotemporal dementia and progressive supranuclear palsy, for instance, the "spikes," comprised of microtubule associated protein tau (MAPT), that normally stabilize and secure these rails tend to fall apart.
This discovery would not have been possible without a consortium of international researchers including co-authors from Canada, France, Japan, Turkey, and the United Kingdom, says Dr. Wszolek, who established the collaborative network of scientists.
Perry syndrome was first described in two unrelated Canadian families in 1975. In a study published in 2007, Dr. Wszolek, along with Swiss neurologist and visiting fellow Christian Wider, M.D., summarized the clinical features of the disease, which include early-onset parkinsonism (stiffness, slowness and rigidity), depression, severe weight loss, and increasing difficulty in breathing. Once symptoms occur, typically in the patient's mid-40s, the disease is rapidly progressive and fatal.
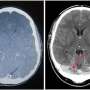
In a subsequent study published in August 2008, the consortium reported that eight patients who died from the disease had substantial loss of neurons in the midbrain area known as the substantia nigra. They also found a molecular signature of Perry syndrome — "inclusions," or clumps, of a protein known as TDP-43 — which is found in patients with frontotemporal dementia or with motor neuron disease. What these clumps represent is not known, says co-author and neuropathologist Dennis Dickson, M.D. "But they are clearly a marker of the disease process in all of these disorders, suggesting a common process is perturbed," he says.
Mayo geneticists hypothesized that Perry syndrome may be caused by mutations within the same gene, even though families afflicted with this disorder are unrelated, and come from different continents. The disease is autosomal dominant, meaning that the chance of inheriting the disease is 50 percent if one parent carries a copy of a mutant gene. With the help and participation of eight families with Perry syndrome, the Mayo-led team set out to find the defective gene.
They determined that each family had one of five novel mutations in the DCTN1 gene, whose protein produces a large subunit of the dynactin complex known as p150glued. This protein is essential to the movement of cargo along the microtubule rails. "Curiously, the mutations all cluster in the p150glued cytoskeleton-associated protein glycine-rich domain and its 'GKNDG' binding motif," Dr. Farrer says. "This region acts like a parking brake, so Perry mutations in p150glued mean that this brake is affected. It would be analogous to driving that train with faulty brakes."
What amazed the researchers are the similarities that Perry syndrome shares with other neurodegenerative diseases. Perry mutations in DCTN1 are physically very close to a mutation previously reported in familial motor neuron disease, they say.
The deposits of TDP43 are also the same as found in motor neuron disease and in some forms of frontotemporal dementia, although they are in a different part of the brain. "With the discovery of mutations in Perry syndrome, researchers have a new means to explore the breakdown in the microtubule transport system in each of these diseases," says Dr. Farrer. "The insides of neurons are very dynamic. Molecules and organelles are constantly being moved to where they are needed, so it makes sense that these disorders, with aging, may be caused by a progressive breakdown in this transport system."
Understanding Perry syndrome may shed light on depression as well as metabolic syndromes, says Dr. Wszolek. Many of the patients have profound depression and about one-third of those commit suicide. Many of the patients also experience severe weight loss and sleep deprivation.
Source: Mayo Clinic